Diabetes – it’s a disease that many Americans have. In fact, according to the Centers for Disease Control and Prevention, more than 100-million U.S. adults have diabetes or prediabetes (which can lead to diabetes if left untreated). The report says that as of 2015, a whopping 9.4-percent of the country’s population is diabetic.
The report focuses largely on type 2 diabetes, which is commonly referred to as adult onset diabetes and is tied to lifestyle and diet (among other risk factors). However, there’s also type 1, which affects patients from a typically younger age. Let’s take a closer look to separate the differences between these two types…
About Type 1
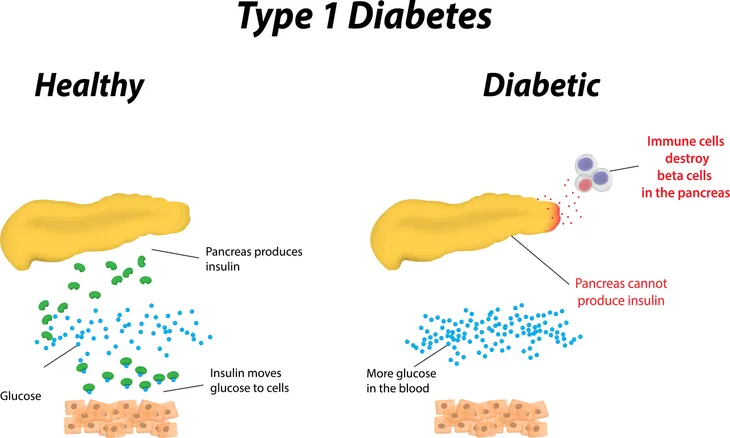
The Mayo Clinic says this form of diabetes was once known as juvenile diabetes due to its root cause – the pancreas does not produce enough of the hormone that regulates the amount of glucose in the blood.
This is a chronic disease that can also develop later in life, and is not directly tied to dietary or lifestyle factors like type 2 diabetes is, adds the source. However, treatment can involve managing lifestyle to minimize its effects.
About Type 2
This is largely the predominant type of diabetes in the U.S., says WebMD. Although patients with type 2 produce the hormone that regulates blood glucose from their pancreas, “their cells don’t use it as well as they should,” it adds.
The pancreas goes into overdrive to try to manage the blood glucose in these patients, but “eventually it can’t keep up, and the sugar builds up in your blood instead,” adds WebMD. Obesity is often blamed for the development of this type of diabetes, but it’s not the only risk factor.
Comparing the Two Types
Diabetes.co.uk breaks down the differences between the 2-types. Here are the highlights: type 1 is usually diagnosed in childhood, while type 2 is usually diagnosed in 30-plus year olds. Type 1 is not linked with excess body weight, whereas Type 2 is.
Type 1 patients usually have higher than average ketone levels (produced by breaking down fat) at diagnosis, while those with type 2 generally have high blood pressure or high cholesterol readings at diagnosis. Type 1 is treated with injections, while type 2 is initially not treated with any medication, it adds. While type 1 patients will need injections for life, type 2 patients may be able to come off diabetes medications in some cases, it adds.
Comparing Symptoms
EveryDay Health says while both types of diabetes can present similar symptoms, there can be some subtle differences. Type 1 can include thirst, hunger, fatigue, frequent urination, weight loss, or even tingling and numbness in the feet and blurred vision when blood sugar is too high, it explains.
Type 2 symptoms often don’t show up right away – “meaning the disease can ravage a person’s body without them realizing it,” it adds. However, early symptoms can be the same as type 1, as well as erectile dysfunction in men and pain in both hands and feet.
Causes of Type 1
Healthline says type 1 is an autoimmune disease – noting the body’s immune system mistakes healthy cells for invaders. “The immune system attacks and destroys the hormone-producing beta cells in the pancreas,” it adds.
Because of this process, the body is no longer able to produce the hormone that regulates the amount of glucose in the blood. The reason this immune response happens isn’t known, but it “may have something to do with genetic and environmental factors, like exposure to viruses,” it adds.
Causes of Type 2
The same source says when it comes to resistance, “Researchers aren’t sure why some people become [resistant] and others don’t,” but there can be contributing factors such as excess weight and not being active (sedentary lifestyle).
There could be genetic and environmental factors involved as well, notes the source. But it comes down to the body not being able to regulate the amount of glucose in the blood properly, even when the pancreas tries to compensate by producing more hormones, it adds.
Risk Factors for Type 1
While the causes for both types are a bit murky, there are some clearly identified risk factors associated for both. In the case of type 1, unfortunately these risk factors can’t be controlled.
For example, Healthline notes that family history, age (mostly children and adolescents), and genetics all play a role in how likely you are to develop type 1 diabetes. Geography also plays a role. “The prevalence of type 1 diabetes increases the farther away you are from the equator,” it notes.
Risk Factors for Type 2
Meanwhile, the list of risk factors for type 2 is long. Healthline lists being overweight or obese (with a lot of belly fat), being physically inactive, having an immediate family member with type 2 as big red flags when it comes to chances of developing type 2.
Other risk factors include giving birth to a baby that’s more than 9-pounds, having gestational diabetes (a type of diabetes that occurs during pregnancy), or being over the age of 45. It also seems to favor some races more – the source says having African-American, Hispanic or Latino American, American Indian, or Alaska Native background will increase risk.
Diabetes Diagnoses
EveryDay Health explains the tests for both types of diabetes are similar. Tests including a blood test to measure fasting blood sugar, as well as a hemoglobin A1C test (measuring average blood sugar over the previous few months), and a glucose tolerance test to see how much blood sugar levels are affected by a sweetened drink.
However, in the case of type 1, doctors can look for antibodies in the blood that attack the hormone-producing cells in the pancreas, it adds. Type 2 diagnoses are more based on symptoms and risk factors, it adds.
Diabetes Diets
In the case of type 1, the goal is to maximize nutrition while monitoring the intake of carbohydrates, proteins, and fats, notes Healthline. “However, there’s no single universal diabetes diet. It involves being mindful of how you eat and how your body will respond to certain foods,” it adds. This could mean enlisting the help of a doctor or dietician.
Meanwhile, the diet for type 2 “is the same diet just about everyone should follow,” it explains. That means choosing a variety of foods high in nutritional value and low in “empty calories,” while controlling portions and eating snacks and meals on a set schedule (to avoid fluctuating blood sugar). Look for veggies, fruits, and whole grains – as well as fish – while avoiding processed meats, sugary drinks, salty or fried foods, and shortening or stick margarine, says Healthline.
Treatment for Both Types
If you have type 1 diabetes, you’ll need a steady regimen of injections or a pump, explains WebMD. You’ll also have to monitor your blood sugars several times each day, it adds. Your doctor will want to see you often to check for any signs of complications. In some cases involving diabetic ketoacidosis (a dangerous blood chemical imbalance), you may be admitted to the intensive care unit, it adds.
The same source says the “treatment for type 2 diabetes will change over time to meet your needs,” but will always involve controlling blood sugar to avoid any complications that can affect the eyes, kidneys, heart, blood vessels and nerves. Your doctor may prescribe certain diabetes medications (short-term or long-term).
Preventing Diabetes
Unfortunately, in the case of type 1, there’s no cure and there isn’t really anything you can do to significantly lower your risk of developing it. But that’s not the same story with type 2 – there are a number of factors within your control that can help you manage or avoid the disease altogether.
The National Institute of Diabetes and Digestive and Kidney Issues says when it comes to lowering your chances of developing type 2, you can plan to lose weight and keep it off, get moving more often (working up to at least 30-minutes of physical activity 5-days a week), and eat healthier foods in smaller portions. Swap your sweet drinks with water, it adds.