A hysterectomy (the removal of the uterus) is, no doubt, a major surgery. With that being said, it should come as no surprise that the recovery will take time, and the patient will experience quite a bit of postoperative pain as they heal. Ahead of this procedure, here’s a look at what to expect following a hysterectomy…
Hospital Stay
Patients who undergo an abdominal (in which the uterus is removed via an incision in the lower abdomen) or radical hysterectomy (where your cervix, parts of the vagina, and lymph nodes are removed along with the uterus, a surgery used only to treat cancer) can expect a hospital stay of at least 2 to 3 days.
Less intensive vaginal (where the uterus is removed via an incision in the vagina) or laparoscopic or robotic (the uterus is removed in pieces via the abdomen with a scope) hysterectomies will require at least an overnight stay.
Prescription Painkillers
Your doctor will recommend prescription pain relief following such a major surgery in order to dull pain and give the body the best opportunity to heal. Keep in mind that with an abdominal hysterectomy your incision scar will eventually heal, but it will probably leave a scar.
Insertion of a Catheter
A catheter is oftentimes inserted following a hysterectomy to facilitate urination for the following 24 hours after surgery. However, it’s important to get up and get moving as soon as you can in order to regain strength and prevent blood clots in your lower legs.
Sanitary Feminine Pads
Vaginal bleeding will occur for several days to a week (spotting) following your hysterectomy, particularly if you have a vaginal incision. The use of sanitary pads will keep you and your underclothes clean, and prevent any embarrassing leaks. Keep in mind that wearing tampons is not recommended during this time.
Also, keep a close eye on the bleeding. If it is as heavy as a menstrual period or extremely consistent and persistent, inform your doctor.
Rest & Recovery
While your doctor will encourage you to move around and do gentle exercise (such as going for short walks) in the weeks following surgery, any movement that has you straining or lifting heavy objects (i.e., shoveling snow, vacuuming, or picking up kids or pets) is not recommended, as it may reopen your surgical incision.
Likewise, you will have to refrain from having sex for a minimum of six weeks.
Hormone Replacement Therapy
One major concern for women who have their fallopian tubes and ovaries removed is the quick plunge into menopause and the associated hot flashes, irritability, and vaginal dryness. Your doctor may recommend hormone replacement therapy to soothe menopausal symptoms (and offer the body estrogen) following your hysterectomy. This is a very personal choice, and you should talk to your doctor in-depth about your options.
WebMD notes that there are also some non-hormonal treatments available. For example there is “Effexor [generic name venlafaxine] and other SSRI [selective serotonin reuptake inhibitor] antidepressants, clonidine (a blood pressure medication), and Neurontin (generic gabapentin, which is prescribed for seizures and chronic pain) have been found to be effective in treating hot flashes.” Again, talk to your doctor to find out what may work best for you.
A Sense of Loss
Some women feel fine after their hysterectomy, but a large portion of women go through a mourning process as they adjust to their new body. A hysterectomy can come with some major changes, the most obvious being the inability to conceive. Not surprisingly, this can have a profound effect on a woman’s mental health, especially those who’ve not had their own children yet or still have a desire to bear their own children.
In addition, some women undergo a hysterectomy due to an illness, such as cancer, which in itself is an additional struggle. There’s also the fact that many premenopausal women begin to enter early menopause due to the removal of their ovaries. All of these obstacles are life altering, so they require some time to adjust and accept. If you’re having trouble with any of these emotions, consider joining a support group or talking to other women who’ve been through or are going through menopause.
Pelvic Weakness
Some women experience pelvic weakness after undergoing a hysterectomy. “If you had some pelvic weakness before surgery, it may get worse afterward leading to bladder or bowel problems,” writes WebMD. The same source also advises doing Kegel exercises to help strengthen the pelvic muscles, which will also help control urinary incontinence.
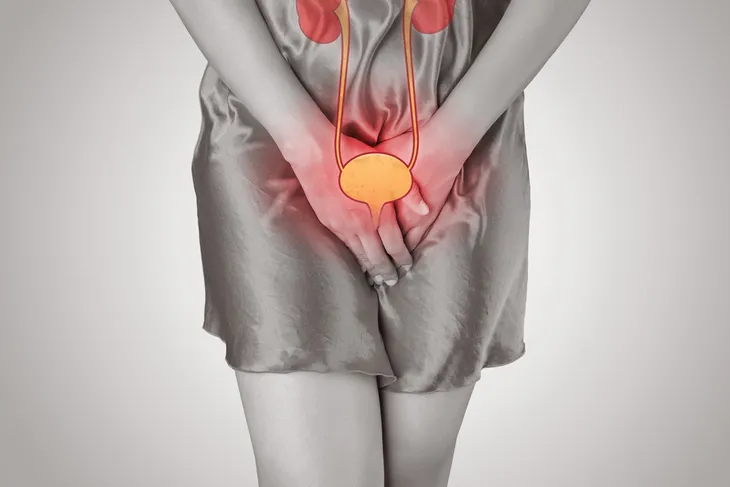
Bowel and Bladder Disturbances
As previously mentioned above, there can also be the concern for bowel or bladder disturbances. According to Everyday Health, bowel and bladder incontinence after a vaginal hysterectomy is not common, but it can happen. One of the causes behind urinary incontinence following a hysterectomy is physical stress which can result from laughing, sneezing, or lifting objects. “This may result from a weakening in the pelvic floor or loss of normal function of the sphincter (the muscle that keeps the urethra closed).
Although this would be more common after a radical hysterectomy for uterine cancer, it may theoretically occur after vaginal hysterectomy as well,” writes the source. Another cause could be because the bladder is overactive as a result of the surgery or a fistula (an abnormal connection between tissues or organs) was created during surgery. These are all highly uncommon, but if this happens to you, seek medical attention right away.
Change in Sex Life
Many women worry that a hysterectomy will affect their sex life. For example, they might fear that sex is no longer pleasurable or that their partner will no longer find them attractive. Both of these worries are just that – worries! According to the Mayo Clinic, if your sex life was healthy prior to the surgery, it will likely return back to normal. Some women even experience more pleasure after a hysterectomy. “This may be due to relief from the chronic pain or heavy bleeding that was caused by a uterine problem,” writes the source.
It is important to note that there is also a chance you’ll experience some discomfort during intercourse after having a hysterectomy. This could be due to the onset of menopausal symptoms, such as vaginal dryness. If this is the case, WebMD advises trying different positions, using lubricants, or even trying a low-dose of vaginal estrogen cream. If you’ve had a hysterectomy and are experiencing low libido or discomfort with sex, talk to your doctor and discuss it openly with your partner to generate some possible solutions.
Post-Op Check-Ups
Of course, your doctor will expect to see you in the weeks and months following surgery to ensure that your surgical incision is healing properly and to answer any questions and concerns you may have associated with the healing process, as well as lifestyle changes after surgery.
Annual Pap Smears & Pelvic Exams
Just because you’ve had a hysterectomy, does not mean you will be excused from annual Pap smears and pelvic exams. It is in your best interest to continue these on an annual basis, minus the Pap smear if your cervix has been removed. Yearly pelvic exams and mammograms are a small inconvenience to pay in order to remain healthy and cancer-free.