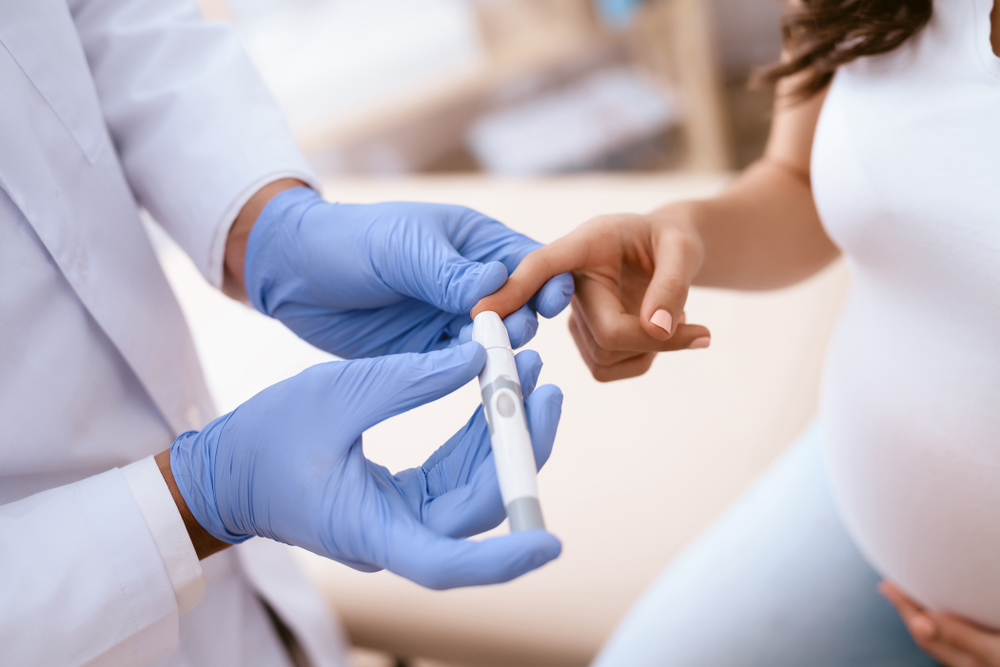
Gestational diabetes is a type of diabetes that begins in late pregnancy as the baby is still developing. The condition strikes approximately 7 to 9-percent of expecting women with elevated blood glucose (or sugar) levels who have never had other forms of diabetes (type 1 and type 2 diabetes).
Here are eight facts to help pregnant women understand pregnancy-related diabetes…
What is Gestational Diabetes?
Gestational diabetes is a condition that strikes during pregnancy. Suddenly mom is unable to produce and utilize the insulin required for a healthy pregnancy so the pancreas overproduces the hormone that regulates glucose in the blood. As a result glucose (or sugars) are unable to convert into energy and they build up to dangerous levels in the blood, a condition known as hyperglycemia.
What Causes Pregnancy-Related Diabetes?
Although the exact cause of gestational diabetes is unknown, the US Centers for Disease Control and Prevention point to insulin resistance as one potential culprit—if elevated hormone levels from the placenta impair insulin, sugar levels may remain in the blood and not be converted into the vital energy needed. Pregnant women can require triple the insulin compared to women who are not expecting.
Will My Doctor Screen for Gestational Diabetes?
Yes, in fact, most physicians will screen for pregnancy-related diabetes around the 28th week of pregnancy as the condition tends to develop anywhere amid the 24 and 28 week mark. The test will examine mom’s blood for elevated blood sugars that occur when insulin hormones are impaired (or not converting blood sugar into energy).
Is the Test Painful?
Not at all. Every pregnant woman is screened for gestational diabetes around 28 weeks, whether they have glucose in their urine or not. Glucose in the urine is common and not necessarily a sign of diabetes. The test will be administered like this:
- Your doctor will ask you to drink a sugary liquid.
- You will wait approximately 1 hour.
- Your doctor will take a small sample of blood to test it for increased blood sugar levels.
- You may also be asked to take a follow up 3-hour glucose to diagnose gestational diabetes. This is only done on patients if the one hour is elevated.
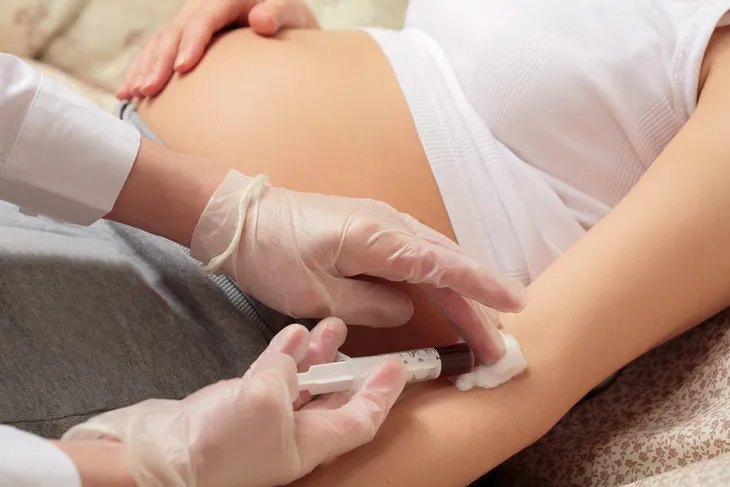
What Puts Certain Pregnant Women at Risk Over Others?
Doctors are extra vigilant with expectant mothers who have a history of pregnancy-related diabetes (with a previous baby), as well as overweight, obese, and older pregnant women who are more prone to developing the condition.
What Are the Symptoms of Gestational Diabetes?
Vast majorities of moms-to-be with gestational diabetes show zero symptoms. However, common signs can include a combination of frequent urination, sudden snoring, extreme and unquenchable thirst, and lethargy.
Can Gestational Diabetes Harm My Baby?
Elevated levels of the hormone that regulates glucose in the blood and blood glucose levels in mom’s body will ultimately cause raised production and high blood glucose levels in the baby’s body as the fetus attempts to expel the excess blood glucose. Basically, baby will be receiving far more energy than her or she requires for growth and the excess energy will be stored as fat, leading to an oversized baby (a condition called Macrosomia), which can cause all sorts of issues during delivery—like injured shoulders, respiratory issues—as well as following birth—such as jaundice, low blood glucose levels, obesity, and the onset of type 2 diabetes.
Treatment for Gestational Diabetes
If you are diagnosed with gestational diabetes, you can still have a healthy pregnancy and a healthy baby as long as the condition is treated, controlled, and monitored closely. The goal will be to decrease blood sugar levels in both mom and baby to prevent issues like obesity and the development of type 2 diabetes down the road.
Mom’s can do their part by exercising regularly, eating well, and maintaining a healthy body weight (before and during pregnancy) in an attempt to maintain safe and balanced blood sugar levels.