Stroke is a leading cause of death and disability in North America. It is a medical emergency. Researchers estimate every year approximately 500,000 Americans have a first stroke and approximately 20-percent die within 30-days. The two types of stroke are ischemic stroke and hemorrhagic stroke. The most common type of stroke is ischemic (85-percent) and occurs when the artery that supplies oxygenated blood to the brain becomes blocked by a blood clot. Hemorrhagic strokes occur when an artery in the brain leaks blood or ruptures, which can damage brain cells by exerting pressure.
Ten risk factors for stroke are…
1. Prior Stroke or Transient Ischemic Attack
Having a stroke puts an individual at increased risk for having another, or recurrent, stroke. The National Stroke Association estimates at least 25- to 35-percent of Americans who have a stroke each year will have a recurrent stroke within their lifetime. Within 5-years of an initial stroke, the risk for recurrent stroke can increase more than 40-percent. Within 5-years of a stroke, 24-percent of women and 42-percent of men will experience a recurrent stroke.
A transient ischemic attack, also referred to as a mini-stroke, may have the same symptoms as a stroke, but the symptoms resolve in minutes to hours (usually less than 24 hours). Symptoms may include weakness, trouble speaking, vision problems, headache, and dizziness. TIA is a medical emergency because it puts individuals at increased for stroke. According to the National Stroke Association 40-percent of individuals who have a TIA will have an actual stroke. Nearly 50-percent of all strokes occur within a few days after TIA.
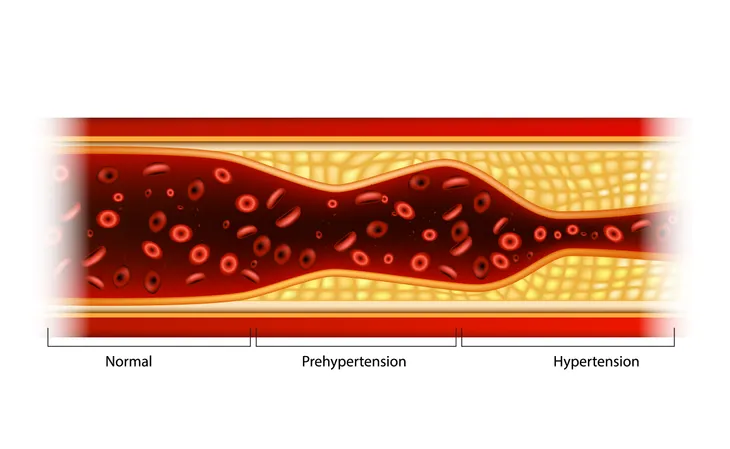
2. Hypertension
Hypertension, also known as high blood pressure, is a major risk factor for stroke. An article published in Hypertension reports the condition affects approximately 43-million individuals in the United States. If an individual is older than 60-years, hypertension is defined as a blood pressure greater than 150/90 mm Hg. If an individual is younger than 60-years, hypertension is defined as a blood pressure greater than 140/90-mm Hg. An article published in the Archives of Internal Medicine reports less than 30-percent of those being treated have blood pressure lower than 140/90-mm Hg.
Hypertension is the most common and modifiable risk factor for stroke. The treatment of hypertension reduces the risk of stroke. An article published in Lancet reports that a decrease in diastolic blood pressure of 5- to 6-mm Hg reduces the risk for stroke by 42-percent. The Systolic Hypertension in the Elderly Program (SHEP) study shows treatment of isolated systolic hypertension in the elderly decreases the risk for stroke by 36-percent.
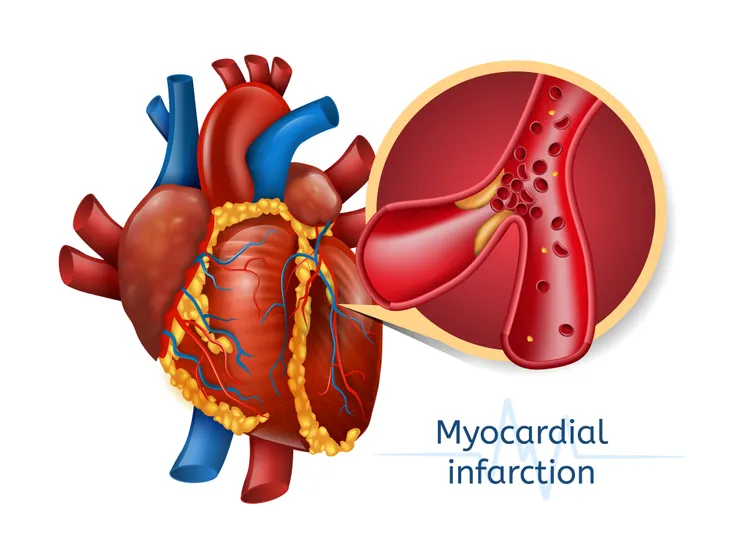
3. Myocardial Infarction
Myocardial infarction (MI), or heart attack, is a major risk factor for stroke. It is directly related to and caused by atherosclerosis, which is the hardening of arteries with cholesterol-like plaque. An article published in Chest reports the incidence of ischemic stroke is approximately 1- to 2-percent per year after MI. An Israeli clinical trial concluded the risk for stroke is greatest in the first month after MI (31-percent).
Treatment to prevent stroke after MI may include oral anticoagulants (blood thinners) and antiplatelet agents. The oral anticoagulant warfarin (Coumadin) is recommended in individuals after MI with persistent atrial fibrillation, decreased left ventricular function, or left ventricular blood clot. A study done by the American College of Physicians reported a decrease in stroke after MI of approximately 1-percent per year with warfarin. An article published in the Annals of Internal Medicine using the same guidelines suggested aspirin, an antiplatelet agent, reduces the risk for stroke after MI by approximately 30-percent.
4. Diabetes
Diabetes is one of the most common diagnoses in medicine and is an established risk factor for stroke. There are two types of diabetes—type 1 and type 2. In type 1-diabetes, the pancreas does not produce any insulin. Insulin is a hormone that lowers blood glucose levels. In type 2-diabetes, the body’s tissues are resistant to the action of insulin. Both types of diabetes result in high blood glucose levels, or hyperglycemia.
Diabetes is diagnosed when the fasting blood glucose level is equal to or greater than 126 mg/dl. Individuals with diabetes are at increased for ischemic stroke. The American Diabetes Association (ADA) reports individuals with diabetes are 1.5-times more likely to have a stroke than non diabetics. Diabetics are also more likely to have hypertension and hyperlipidemia (high cholesterol), which further increases the risk for stroke. The United Kingdom Prospective Diabetes Study (UKPDS) demonstrated a 25-percent reduction in stroke with more intensive blood glucose control.
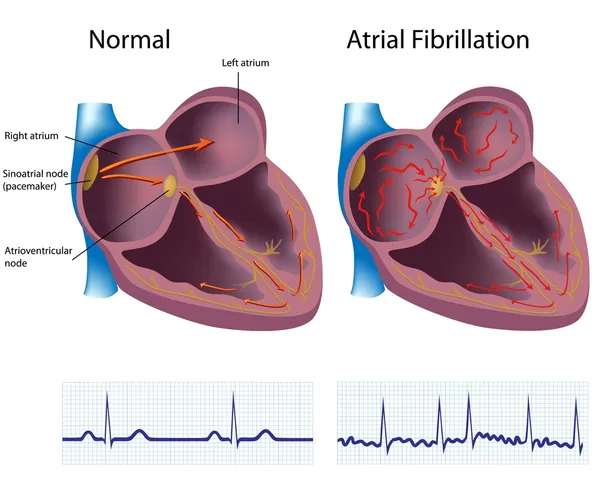
5. Atrial Fibrillation
Atrial fibrillation (AF) is a heart arrhythmia (heart rhythm disorder) that increases the risk for stroke. It affects the upper chambers of the heart, or atria. Instead of contracting effectively, the atria quiver, which can cause the blood to pool and clot. If a piece of clot breaks off, it can wind up blocking an artery in the brain and stopping blood flow. The process is termed ischemia. If ischemia lasts long enough, it can lead to necrosis, or the death of cells, of the brain.
A study published in the Archives of Internal Medicine concluded individuals with AF have double the rate of death than those without AF. The Framingham Heart Study calculated the risk for stroke to be 5-percent per year in individuals with nonvalvular AF. A study published in Chest found individuals with valvular AF have an even higher chance (17-times greater) for stroke than those without AF.
6. Hyperlipidemia
Hyperlipidemia, or elevated levels of blood cholesterol, is an established risk factor for stroke. Cholesterol is a waxy, fat-like substance manufactured in the liver. It is also obtained from the foods we eat. Excess blood cholesterol winds up being deposited in the walls of arteries. Hyperlipidemia refers specifically to elevated levels of total cholesterol and low-density lipoprotein (LDL). LDL is often referred to as “bad cholesterol” due to its role in the development of atherosclerosis, which can lead to coronary heart disease and ischemic stroke.
Statins are a class of medication routinely used to treat hyperlipidemia. Examples of statins include atorvastatin (Lipitor), rosuvastatin (Crestor), pravastatin (Pravachol), simvastatin (Zocor), and fluvastatin (Lescol). A scientific review published in the Journal of the American Medical Association (JAMA) concluded treatment of hyperlipidemia with statins yielded a 25-percent reduction in the risk of fatal and nonfatal stroke. In high-risk individuals, the recommended target LDL is less than 100-mg/dl.
7. Carotid Artery Disease
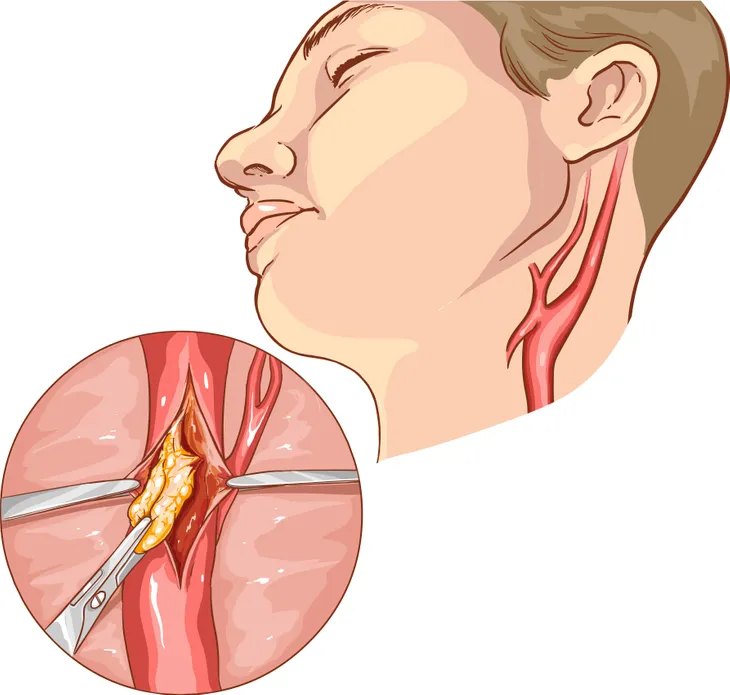
Carotid artery disease is an important risk factor for stroke. The carotid arteries are major blood vessels in the neck that supply blood to the brain, neck, and face. There is a right carotid artery and a left carotid artery. Carotid artery stenosis, or narrowing of the carotid artery, is usually due to atherosclerosis (hardening of arteries with cholesterol-like plaque). Cholesterol plaque in the carotid artery may fragment and travel to the brain causing a stroke.
The risk of stroke increases with the degree of carotid artery stenosis, which can be determined using cerebral angiography (X-rays of the carotid arteries after the injection of contrast). In the Asymptomatic Carotid Atherosclerosis Surgery (ACAS) trial, men with 60- to 99-percent asymptomatic carotid artery stenosis had an absolute reduction for stroke and death of 66-percent when treated with carotid endarterectomy. During this surgery, a cardiovascular surgeon opens the carotid artery and removes the cholesterol plaque.
8. Cigarette Smoking
Researchers have established cigarette smoking as a risk factor for stroke. It causes direct damage to the heart and blood vessels. The nicotine in cigarettes may significantly increase blood pressure (BP). The carbon monoxide in cigarette smoke may reduce the amount of oxygen that reaches the body’s tissues, including the brain. A study published in the British Medical Journal found that stroke risk increases 2-fold among heavy smokers compared with light smokers.
Exposure to secondhand smoke can also damage the cardiovascular system and may even increase a non smoker’s risk for stroke. The use of oral contraceptives combined with cigarette smoking greatly increases the risk for stroke. It’s never to late to quit smoking. A study published in Family Practice found that one-time advice from a health care professional during routine interactions had an appreciable impact on quitting smoking. A clinical trial published in the Journal of the American Medical Association (JAMA) reports the increased stroke risk disappears within 5-years of quitting smoking.
9. Excessive Alcohol
Excessive alcohol consumption may increase the risk for stroke. The United States Centers for Disease Control and Prevention (CDC) report a standard drink is equal to 14-grams of pure alcohol. This amount of pure alcohol can be found in 12-ounces of beer (5-percent alcohol content), 8-ounces of malt liquor (7-percent alcohol content), 5-ounces of wine (12-percent alcohol content), and 1.5-ounces of 80-proof (40-percent alcohol content) distilled spirits or liquor (gin, rum, vodka, or whiskey).
The Dietary Guidelines for Americans defines moderate, or judicious, alcohol consumption as having up to 1-drink per day for women and up to 2-drinks per day for men. A clinical trial from Hawaii found alcohol consumption has a direct dose-dependent effect on the risk for hemorrhagic stroke. A study published in the New England Journal of Medicine proposes a J-shaped relationship between alcohol use and ischemic stroke, which refers to a protective effect in light or moderate drinkers and an elevated stroke risk with heavy alcohol consumption.
10. Heredity
Heredity refers to when members of a family pass traits from one generation to another through genes. A gene is the basic physical and functional unit of heredity. Genes, which are composed of DNA, provide instructions to make molecules called proteins. Every individual has two copies of each gene, one inherited from each parent. The Human Genome Project estimates that humans have between 20,000 and 25.000-genes.
A person’s risk for stroke may be greater if a parent, grandparent, sister, or brother has had a stroke. Researchers at Boston University found that children with parents who had suffered a stroke by 65-years of age were more likely to have a stroke themselves. When controlling for traditional stroke risk factors (such as hypertension, diabetes, smoking, and heart attack), researchers concluded study participants had double the risk of having a stroke at any age and 4 times the risk of having a stroke by 65-years of age.