Nobody wants to get a colonoscopy, however they are the best way to detect and prevent colon cancer. Unfortunately, many people avoid this procedure out of fear of what it might entail or what they have to go through. Although it’s not pleasant, it could be life saving.
Colon and rectal cancers (collectively known as colorectal cancer) are the third most common type of cancer in men and women, and the second leading cause of cancer-related death in the U.S., says Harvard Health.
In order to have a colonoscopy, the colon has to be empty and clean which does require a little bit of prep work. We’re going to walk through some tips on how to prepare for a colonoscopy, including dietary choices, medications, as well as what to expect before, during, and afterward. Let’s take a look…
What Is a Colonoscopy?
A colonoscopy is an exam used to spot colon cancer while it is still treatable or before it has spread to other parts of the body, says Harvard Health Publishing. They can also detect and remove polyps (small growths) or other abnormalities that could potentially develop into colon cancer.
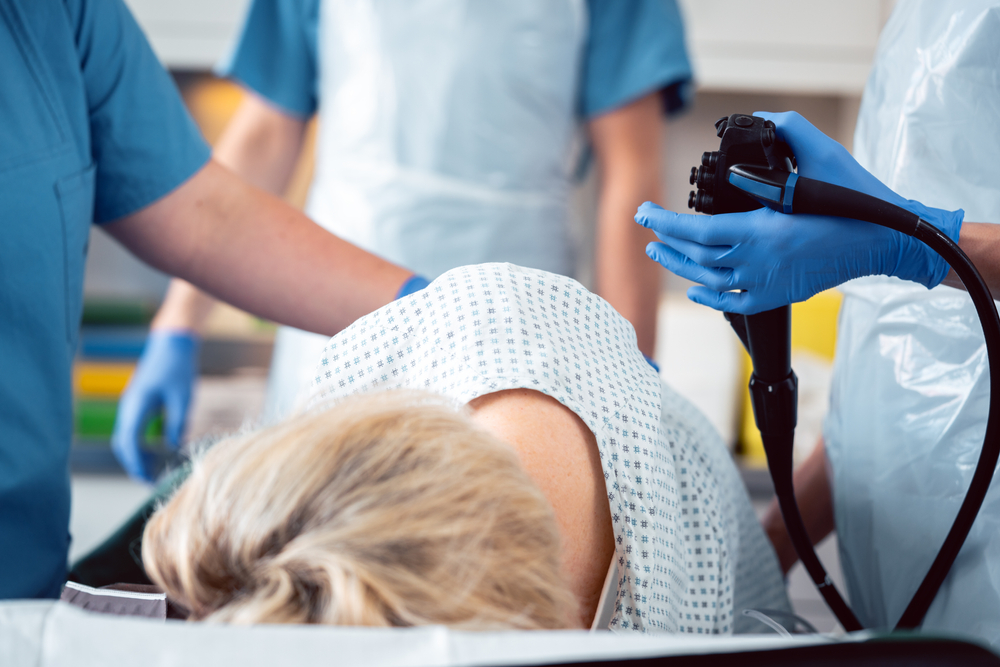
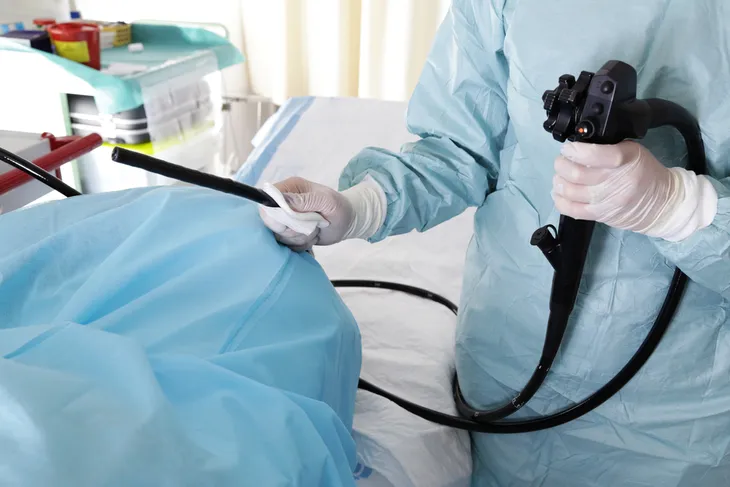
According to the Mayo Clinic, the procedure is performed by using a long, flexible tube (colonoscope) that is inserted into the rectum. Attached is a tiny camera that allows the doctor to view the inside of the colon.
The source goes on to explain that colonoscopies are used to investigate any intestinal problems, such as abdominal pain, rectal bleeding, constipation, diarrhea, or other issues. It’s also used to screen for cancer and look for polyps.
Store-Bought Necessities
Your doctor is the best source of information when it comes to what to do in order to prepare for a colonoscopy. You’ll be provided with step-by-step instructions, however, there are a couple products that might come in handy before and after the procedure.
WebMD recommends having a few key supplies on hand like prescription over-the-counter laxatives (one that is specified by your doctor), moist or medicated wipes, and diaper cream.
Depending on what medical center the procedure is being done, the process of emptying the colon might differ. Some places use a bowel-cleaning fluid while others just rely on diet. Either way, these are the two main strategies.
Eat Low Fiber and Soft Foods
Not surprisingly, diet comes into play in the days leading up to a colonoscopy. You can jump-start the cleaning process by eating light about 3 to 4-days ahead and sticking to low-fiber, easy-to-digest foods that will leave the body quickly.
WebMD suggests white bread, pasta, rice, well-cooked vegetables (without skin), fruit (without skin or seeds), lean meat, chicken, or fish, and eggs.
Foods to Avoid
On the flip side, avoid foods that are more difficult to digest like seeds, nuts, popcorn, fatty foods, tough meat, whole grains, raw vegetables, fruits with seeds and peel, corn, broccoli, cabbage, beans, or peas.
Ask About Medications
Provide the doctor with a list of any current medications at least a week before the exam, says the Mayo Clinic. This is especially true for people who are taking aspirin or blood thinning medications. You might need to adjust the dose or stop taking them temporarily.
You’ll likely need to also stop taking vitamins and other supplements, says WebMD.
The Day Before…
Fasting begins the day before a colonoscopy which means strict dietary limitations. You can’t eat anything solid and only consume clear liquids, explains WebMD.
You’ll need to drink lots of water or clear liquids like sports drinks, clear juice (apple or white grape), and clear broth. You can drink coffee and tea, but without cream. According to WebMD, gelatin and ice pops are okay, but nothing with color. The dye can discolor the lining of the colon and make it harder to see during the procedure. You should also avoid alcohol and colored drinks like milk and orange juice.
Stop eating and drinking anything, even liquids, two to four hours ahead of the procedure. Your doctor will provide exact instructions on that.
The Night Before…
The night before a colonoscopy is where the majority of the prep work comes into play. Depending on the doctor, the exact prep differs based on what they prefer, as well as the time of the colonoscopy and any previous experience, says Harvard Health.
You’ll likely be advised to take some strong laxatives that will help clear out the digestive tract, says WebMD. This is a method called split dosing. “You’ll drink a half-gallon of liquid laxative in the evening. Then you’ll get up about 6 hours before your appointment to drink another half-gallon,” writes the source.
Here are some tips from WebMD on how to make drinking the solution more bearable:
- Try mixing with something flavored (i.e. sports drink or powdered drink mix)
- Keep it cold
- Drink through a straw and place the straw at the back of your tongue
- Follow it up by eating or drinking something flavorful
- Suck on a lemon slice or piece of hard candy
When the laxative takes effect it will likely cause frequent diarrhea, along with some cramps and bloating. If you have hemorrhoids, they’ll likely become irritated. You might feel nauseated and even vomit. If this is the case, take a short break.
To make the process a little easier, stay in the bathroom and bring a book. Apply diaper cream before the diarrhea starts and use moist or medicated wipes to clean afterward. If the laxatives work properly, by the end your stool will look like urine or clear water. This means the process is complete.
What to Expect During
The prep is the worst part as the procedure itself only takes 30 to 60-minutes. You’ll be sedated and wearing a gown. The sedation can be provided either in pill form or through IV. This is just to minimize any potential discomfort.
Lying on your side with knees drawn up to the chest, the colonoscope is inserted into the rectum. This scope is the entire length of the colon and contains a light and tube that pumps air or carbon dioxide into the colon. “The air or carbon dioxide inflates the colon, which provides a better view of the lining of the colon,” writes the Mayo Clinic.
You might have some abdominal cramping or feel the urge to have a bowel movement when the scope is removed.
It also contains a tiny video camera at the tip which sends images to an external monitor so the doctor can study the inside of the colon. “The doctor can also insert instruments through the channel to take tissues samples (biopsies) or remove polyps or other areas of abnormal tissue.”
What to Expect Afterwards
While the procedure isn’t major and has patients in and out the same day, it does take about an hour to recover from the sedative and requires assistance getting home. Please arrange for a ride home prior to the exam. Do not drive.
If a polyp was found during the exam, a temporary special diet may be required, notes the Mayo Clinic.
You’ll likely feel a little bloated and gassy afterwards. The Mayo Clinic suggests walking to help relieve any of this discomfort. You might also notice a small amount of blood in your first bowel movement afterwards. This usually isn’t concerning, unless it persists or there is any abdominal pain, fever, or blood clots. “While unlikely, this may occur immediately or in the first few days after the procedure, but may be delayed for up to one to two weeks,” writes the source.
The Results
What’s nice about a colonoscopy is that the results of the exam are provided almost immediately. A negative result means nothing was found in the colon (i.e. no abnormalities).
For those with a negative result and no risk factors for colon cancer other than age, you’ll be recommended to come back for another one in 10 years, says the Mayo Clinic. If there’s a history of polyps, a colonoscopy is recommended every 5 years. If the exam was unsuccessful due to residual stool, you’ll have to come back the following year.
A positive result means there were polyps or abnormal tissue in the colon. The Mayo Clinic explains that most polyps aren’t cancerous, but they can be precancerous. If any are found, they’re removed during the exam and sent to a laboratory for analysis.
Any follow up surveillance or treatment will depend on the size and number of polyps.