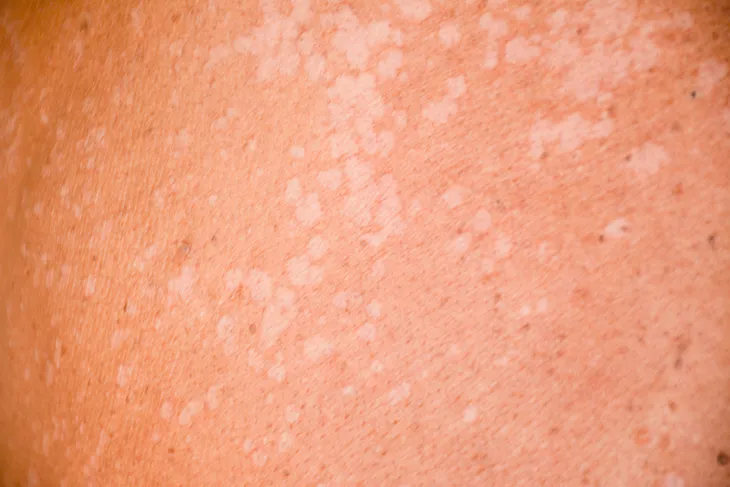
Tinea versicolor, also called pityriasis versicolor, is a fungal infection of the skin. It is one of the most common skin infections in tropical and subtropical climates but it can also happen to anyone, including healthy people. The fungus that causes this infection occurs naturally on the skin but if it grows out of control, it can cause a fungal infection.
Thankfully, tinea versicolor can often be treated at home but in some cases, it’ll need to be treated by your doctor. Before treatment, you’ll want to have an understanding of what the infection looks like, what causes it, and how to diagnose it. In this article, we learn everything there is to know about tinea versicolor including the signs, causes, and treatment options available. Let’s explore these next!
Signs and Symptoms of Tinea Versicolor
There are several signs and symptoms you’ll want to look out for that indicate you may have tinea versicolor. The most common sign is patches of skin discoloration, which is typically referred to clinically as hypopigmentation. These commonly appear on the neck, chest, back, and upper arms.
The Mayo Clinic explains the patches can appear white, pink, red, or brown. They can also be lighter or darker than the skin around them. These spots also don’t typically tan the same way the rest of your skin does and may even show up more boldly when you do tan your skin.
Finally, another sign of a tinea versicolor is dry scaly patches. They may even itch or hurt, however, this symptom is more rare.
Other Skin Conditions That Look Like Tinea Versicolor
A few skin conditions have similar symptoms and may be mistaken for tinea versicolor. This includes vitiligo and pityriasis rosea.
Vitiligo is a disease that makes your skin lose color (a process known medically as depigmentation), and while it can look similar to tinea versicolor, some of its symptoms differ. For starters, vitiligo is not caused by a fungus and doesn’t change your skin’s texture. It also typically appears on the mouth, eyes, groin, armpits, fingers, and wrists. Finally, vitiligo often presents itself as symmetrical patches.
Secondly, pityriasis rosea is also similar but usually appears in the shape of a Christmas tree on your back. It often starts as a “herald patch,” a round or oval scaly patch or plaque that appears several days or weeks before the rash. Fortunately, it’s not harmful or contagious.
Causes of Tinea Versicolor
Tinea versicolor is a fungal infection of the skin and is caused by too much growth of yeast. The yeast that causes the infection is called Malassezia, which grows on normal, healthy skin. Certain things can trigger the overgrowth of this type of yeast and ultimately cause the infection. These include:
- A weakened immune system
- Living in a hot climate
- Having oily skin
- Sweating often
- Hormonal changes
Is Tinea Versicolor Harmful or Contagious?
Thankfully, since the yeast that causes this infection naturally grows on your skin, tinea versicolor is not contagious. It can affect anyone, although it’s more common in teens and young adults.
Tinea versicolor isn’t usually painful. That said, it may cause emotional distress. Some people even feel self-conscious about the infection.
How to Manage Tinea Versicolor
Tinea versicolor cannot be spread from person to person (i.e., it is not contagious), but there are things you can do to help manage it and prevent it from spreading on your body.
For starters, avoid oily skin products and wear loose-fitting clothing. You should also reduce the time you spend in the sun, as it can make the infection more apparent. When you do go outdoors, make sure you put on sunscreen.
Risk Factors for Tinea Versicolor
Unfortunately, tinea versicolor can affect healthy people. That said, several factors can put you at a higher risk of developing this infection such as a family history of the skin infection.
Other risk factors include heat and humid climates, diabetes, pregnancy, some types of cancer, excessive sweating, and having a weak immune system. Some medications that weaken your immune system can put you at greater risk too.
When to See a Doctor
Tinea versicolor can sometimes be treated at home using over-the-counter (OTC) antifungal medications. However, if at-home treatments are not effective you should see your doctor. You should also see your doctor if the fungal infection returns after going away and if the patches cover large areas of your body.
Diagnosing Tinea Versicolor
To diagnose tinea versicolor, your doctor will start by examining your skin and looking at the patches. If they can’t confirm a diagnosis by examining your skin, they may take a skin scraping. This is done by scraping the skin gently to remove cells. The cells are then examined under a microscope to confirm whether or not they contain the type of yeast that causes this condition.
Your doctor may also need a biopsy or tissue sample of the affected area. Finally, another way they may diagnose tinea versicolor is by using a Woods lamp. This machine uses ultraviolet light to examine the area. It’s typically held about 5-inches from your skin. If your skin appears yellow or green, this confirms that the causative yeast is present.
Treatment Options for Tinea Versicolor
Mild symptoms can be treated at home with OTC antifungal creams and shampoos. However, if at-home treatment doesn’t work, you’ll need to seek treatment from your doctor.
Your doctor may prescribe medications like topical creams for the affected area. They may also prescribe certain pills to help treat the infection.