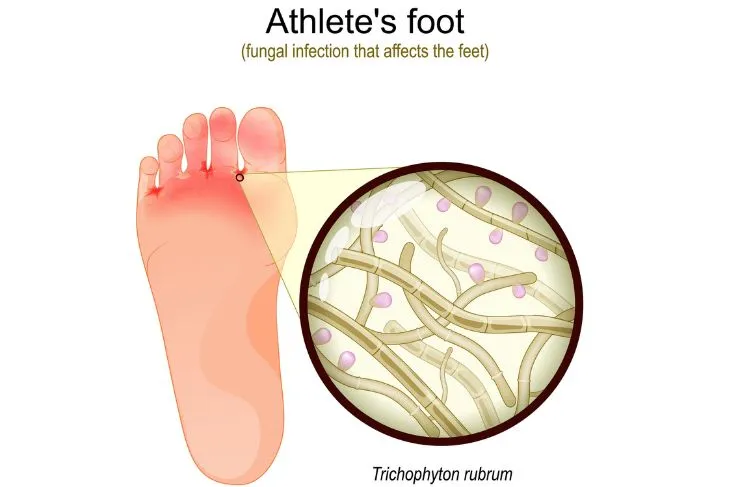
- Athlete’s foot is a fungal infection that occurs on the foot and thrives in dark, moist environments.
- It is caused by the same fungi (dermatophytes) that causes ringworm or jock itch and is spread through contact with an infected person or contaminated surface.
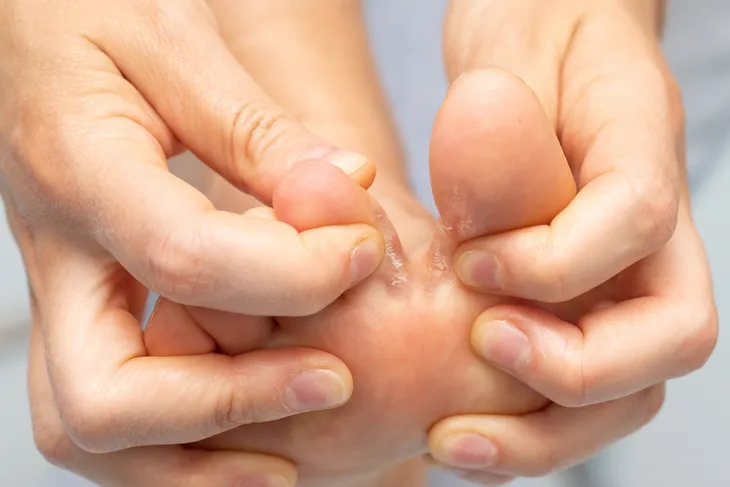
- The most common symptoms are a painful itchy and scaly rash. The skin will thicken, become inflamed, discolored, and may even develop blisters.
- You can treat athlete’s foot with over-the-counter or prescribed medication, even antibiotics if necessary.
Athlete’s foot, also known as tinea pedis (or ringworm), is a highly contagious fungal skin infection that develops on the top outer layer of skin on the foot. The rash most commonly crops up in moist, dark areas, such as between the toes where air can’t promote healing.
Gym showers, swimming pools, locker rooms, and any environment where people are likely to be walking barefoot, are all hot spots for athlete’s foot exposure. The fungus contaminates a surface as it transfers from one infected foot to the next one that comes along. Here’s a look into the types, symptoms, causes, and treatment options, as well as some prevention tips…
Types of Athlete’s Foot
Toe Web Infection
A toe web infection is sometimes referred to as an interdigital infection by doctors. This is basically just a fancy way of saying the infection is between fingers or toes, explains WebMD. It will likely appear between the fourth and fifth (i.e. pinkie) toe. If it does, WebMD warns that sometimes bacteria can take hold and make the infection worse.
One of the telltale signs of a toe web infection is a burning sensation between the toes. “The skin may be red, peeling, or scaly, and the rash may smell or give off discharge,” writes the source. If the infection is extraordinarily bad, it can even make the skin green.
Moccasin Infection
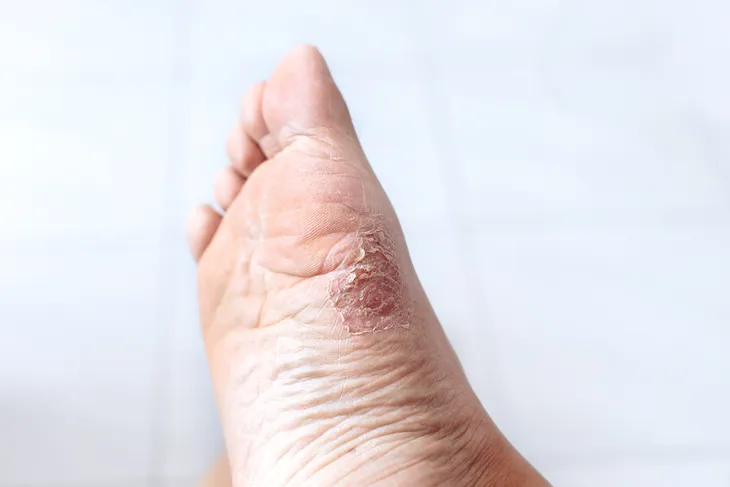
According to WebMD, if the fungus covers the whole sole area of the foot, it’s known as a moccasin infection. In this case, the infection might even spread up the heel and alongside the foot.
If a person has this type of infection, they might not notice it at first. Their feet might just feel sore, dry, or slightly itchy, explains the source. Eventually the skin will thicken and start to crack or peel. “If the infection advances to your nails, your toenails may also get thick and crumbly. Sometimes the nails even come out,” writes WebMD.
Vesicular Infection
Vesicular is the medical term for blisters which is why this type of athlete’s foot was given this name. The signature mark of a vesicular infection is blisters. WebMD warns that if these blisters burst, they could get a bacterial infection and require antibiotics.
This infection can occur anywhere on the foot. “But the small, red blisters usually pop up on your soles or between your toes,” says WebMD. “The rash may feel itchy or painful.” It’s often the worst during the hot summer months.
Ulcerative Infection
This type of infection is quite rare, but it can happen if the infection gets so bad that it develops open sores or ulcers. An ulcerative infection is by far the worst type of athlete’s foot and most painful.
The ulcers that develop are ripe for infection by bacteria which can only be treated with antibiotics. In addition to having open sores, WebMD warns they might ooze a discharge, the skin will become inflamed, and even discolored.
Symptoms
Thickening of the Skin
Athlete’s foot tends to develop as one of the several types we listed above. In the case of moccasin, there will be a thickening of the skin. It causes the skin on the bottom of the heel and sides of the feet to become thick, cracked, and painful.
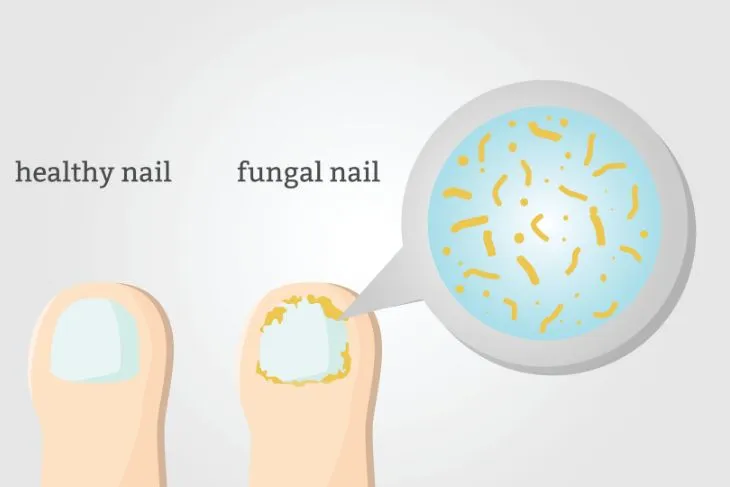
This thickening of the skin will also quickly infect the toenails. They will also thicken and become discolored (yellow or opaque) until they start to disintegrate and crumble. Eventually the toenail will fall off and leave the toes prone to greater infection.
Scaly Rash
Athlete’s foot most often affects the webbing between the toes. This type of athlete’s foot will cause a telltale scaly, peeling rash between the webbing of the toes. A toe web infection is difficult to clear up as the infection focuses on the dark, moist areas of the foot that get little air. Not only that, but it can also quickly spread up the sides of the feet.
The infection worsens if wearing tight shoes and can be particularly painful after removing sweaty shoes. In this case eczema can also appear on the feet making them very itchy and scaly. If the rash does not resolve on its own with over-the-counter (OTC) treatment, see a doctor.
Itchy Feet
The red, scaly rash that’s so indicative of athlete’s foot usually causes extreme itchiness—particularly right between the webbing of the toes. As mentioned, the infection worsens due to too tight shoes and sweaty socks that are left on too long.
This is why itching is at its worst right after shoes and socks are removed. Don’t be tempted to scratch infected areas because the fungal infection can easily spread from foot to hand and to other areas of the body.
Foot Blisters
Foot blisters are indicative of a vesicular infection which causes painful fluid-filled blisters or ulcers to develop on the bottoms of the feet under the skin. These blisters often become red and inflamed, and eventually erupt. Unfortunately, the swelling and eruption of ulcers can happen several times following the initial infection.
A bacterial, long-term infection is more common to vesicular infection type athlete’s foot, and can quickly cause a bacterial infection. Don’t pick at blisters as they can easily spread to the palms, the side of the fingers, and other areas with contact.
Discoloration and Toenail Loss
A moccasin type of athlete’s foot infection affects the skin on the bottoms of your feet (cracking and peeling of the sole) as well as your toenails. You will often notice pain and burning under the toenails first as well as slight discoloration of the nails themselves.
When athlete’s foot infection sets into the toe nails, the affected toenails will thicken, crack, and begin to disintegrate (or crumble away in thick pieces). Eventually the affected nails will break down so much that they will fall away from the nail bed.
Causes of Athlete’s Foot
Athlete’s foot is caused by the same fungi (dermatophytes) that causes ringworm or jock itch, explains the Mayo Clinic. In a clean, dry environment this fungus is harmless, but in damp and moist conditions like sweaty socks or shoes, or warm humid conditions, such as showers and locker rooms, the organism will rapidly multiply.
People often get athlete’s foot by coming into contact with an infected person or touching a contaminated surface (towels, floors, shoes). The Mayo Clinic warns the infection can even spread from the foot to other parts of the body, especially if a person scratches or picks at the infected areas of their foot.
How to Prevent Athlete’s Foot
Athlete’s foot is highly contagious so it might seem hard to avoid it, but there are some steps people can take to protect themselves (and others), especially if they are spending time in areas like swimming pools and locker rooms.
The Mayo Clinic advises letting your feet air out, when possible. You should also wash your feet daily with warm, soapy water. Afterwards, rinse and dry them carefully, especially between the toes. Change your socks regularly (at least once a day) and wear moisture-wicking socks like cotton to help keep them dry. This is important for people whose feet get really sweaty. Another tip from the Mayo Clinic is to alternate shoes each day. This gives them time to dry out between uses.
If you’re in a public place, such as a public pool, shower, or locker room, wear waterproof sandals or shoes. Be mindful of others. People with athlete’s foot should try to limit contaminating other surfaces, especially if they live with others. Don’t share shoes or unwashed bedding and towels.
Athlete’s Foot Treatment Options
While it’s certainly unlucky to get athlete’s foot, it’s not the end of the world. The infection can be treated safely at home with a topical anti fungal cream (i.e. clotrimazole or miconazole). These can be purchased OTC at a local drugstore or pharmacy.
If nonprescription medications don’t work, the Mayo Clinic advises going to see a doctor to get something a little stronger, like a prescription-strength medication. If the infection is severe, they may have to prescribe anti fungal pills or take both a topical and oral medicine.
Your doctor may also recommend soaking infected feet in salt water, tea tree oil (melaleuca alternifolia) and diluted vinegar bath to help dry out the blisters and encourage healing.