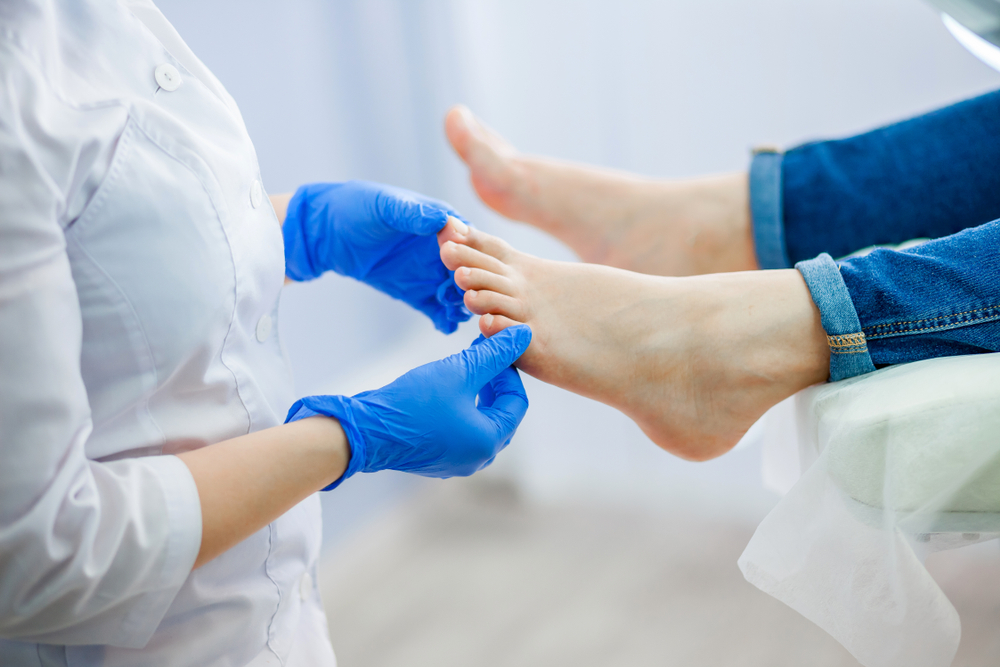
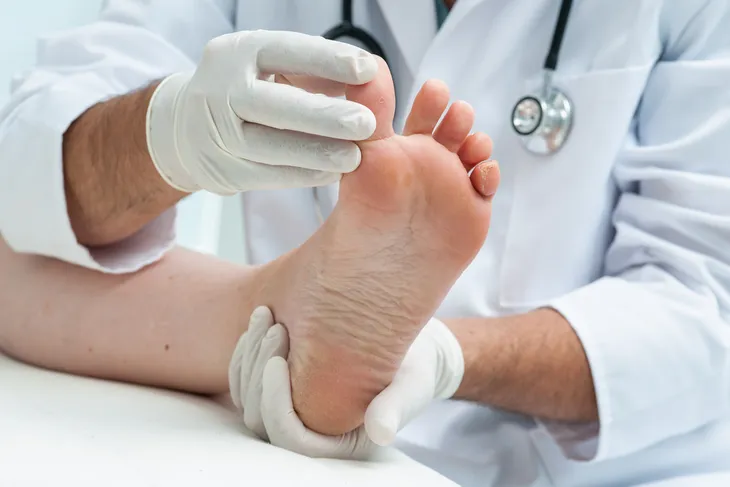
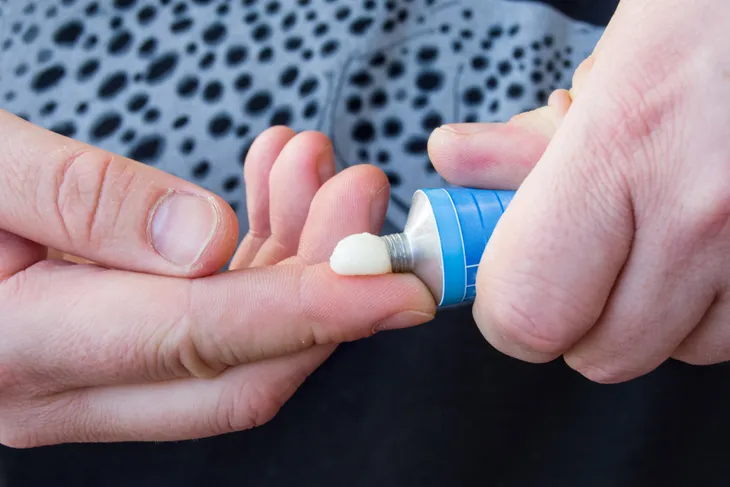
- Paronychia is an infection that affects the tissues surrounding fingernails and toenails (nail folds).
- Causes of paronychia include bacterial or fungal infections, ingrown fingernails or toenails, and physical trauma.
- Paronychia infections can be treated with various remedies, from over-the-counter creams to surgery.
Paronychia is a common infection that develops in the cuticles and skin at the base and sides of the fingernails and toenails. The condition presents as acute or chronic, and studies have shown that it’s more prevalent in women than in men.
In most instances, paronychia is easily treatable, but severe infections can potentially spread to the surrounding bones of the hands and feet and require surgical intervention. Here’s a look at the common signs of paronychia plus how to treat it.
Signs and Symptoms of Paronychia
The most common signs and symptoms of paronychia include redness or inflammation of the cuticle skin and skin surrounding the fingernails. It’s also typically accompanied by swelling and tenderness.
You may also develop pus-filled blisters beneath the nail fold skin or a painful skin abscess. If the infection spreads into the nail itself, it can lead to discoloration and abnormal nail growth. In some cases, the fingernail or toenail may detach from the nail bed, or the nails may become dry and brittle.
What Causes Paronychia?
Paronychia occurs when fungi or bacteria such as Staphylococcus aureus and Streptococcus pyogenes enter the skin and create an infection. Bacteria and fungi can get beneath broken skin via cuts, scrapes, ingrown toenails, and hangnails, and infection can also occur when there is trauma to the cuticles or nailbed.
Nail biting and injuries from manicure or pedicure tools sometimes lead to exposed, broken skin, making it more vulnerable to infection. Frequent handwashing or exposure to chemicals may cause cracks in the skin around the nails, creating a breeding ground for bacteria and fungi. Additionally, chemotherapy drugs and antibiotics are linked to nail infections.
Topical Medications for Paronychia
Paronychia infections can be treated with over-the-counter topical medications such as antibacterial ointments, hydrocortisone creams, and antifungal creams. Antibacterial ointments are formulated to fight existing infections and promote healing, while hydrocortisone creams can help reduce swelling and pain associated with infection. Over-the-counter topical antifungal creams may be beneficial for mild cases of paronychia caused by fungus.
If you’re experiencing symptoms such as severe pain or swelling or if pus-filled blisters have developed around the nail, it’s important to consult a medical professional before attempting to use an over-the-counter topical medication. If the infection has spread to surrounding tissues, your physician may prescribe an oral antibiotic or another type of prescription medication.
Oral Medications for Paronychia
Oral medications for paronychia are generally prescribed to individuals with chronic or severe acute infections. The prescribed medicines can vary depending on whether the condition is bacterial or fungal. Broad-spectrum antibiotics are commonly prescribed for bacterial paronychia infections, and oral antifungal medications are often ordered for individuals with chronic fungal infections of the toenails or fingernails.
If you’re prescribed antibiotics for paronychia, it’s essential to finish the entire course unless otherwise directed by your physician, even if your symptoms immediately improve. Stopping the antibiotic treatment early can cause any remaining bacteria to multiply and potentially cause re-infection.
Medical Procedures for Paronychia
When paronychia infections cause abscesses or pus-filled blisters, your physician may recommend a drainage procedure to remove the harmful bacteria and promote healing. During a drainage procedure, the skin surrounding the nail is treated with a numbing agent before the abscess is opened up with a scalpel and flushed with saline solution.
In cases of fungal paronychia that cause abnormal nail growth, surgical procedures to remove the affected nails and surrounding skin are sometimes considered the best option to completely eliminate the fungus and promote healthy nail regrowth.
Home Remedies for Paronychia
Home remedies often help to eliminate mild cases of paronychia. Soaking the affected finger or toe in warm water can help soften the nail and surrounding tissues, which is helpful when the nails are ingrown or the skin is inflamed. Warm water soaks can also help to drain fluid or pus build-up from beneath the skin. If the infection is caused by a fungus, soaking the nail in antiseptic mouthwash may help hinder fungal growth and eliminate nail discoloration.
Tea tree oil has natural anti-fungal properties that may help treat fungal nail infections and can be applied directly to the affected nails. For best results, it’s recommended to apply the oil at least twice per day.
Is Paronychia Preventable?
While it’s not always easy to avoid unforeseen accidents or other issues that can cause nail trauma and lead to infection, there are several steps you can take to help prevent common types of paronychia. Good hygiene practices such as keeping the feet and hands clean and dry can help eliminate dirt, bacteria, and other impurities from the nail beds.
Wearing gloves when washing dishes or working with harsh chemicals can also protect the skin from irritation. Trimming the fingernails and toenails on a regular basis may aid in preventing overgrown or ingrown nails that can lead to infection, and applying moisturizer after bathing and showering helps prevent dry, cracked skin.
Acute Paronychia vs. Chronic Paronychia
Acute paronychia infections are most often caused by bacteria. They tend to come on suddenly and resolve within a few weeks to a few months. Many acute infections are easy to treat with over-the-counter ointments and home remedies, however, in some cases of acute paronychia, the infection can spread rapidly and require medical intervention.
Chronic paronychia infections are generally caused by a fungus such as Candida (the fungus responsible for most types of yeast infections) or trauma that leads to injury of the nail and nail bed. Chronic paronychia infections tend to develop slowly over time, and the symptoms usually last much longer than those in acute infections. In many cases, chronic infections are treated with prescription medications and/or medical or surgical procedures.
Complications of Paronychia
One of the most common complications of paronychia infection is nail dystrophy, which causes the nail plates to develop grooves and ridges. Nail dystrophy usually occurs with chronic paronychia infections, and the condition is typically treated with antibiotics or antifungal medications.
Acute paronychia infections on the fingers can sometimes spread beyond the nail area and lead to a serious condition called cellulitis. Cellulitis can affect underlying tendons and bones, so you must consult a physician immediately if you experience symptoms such as fever or chills or if the skin surrounding the infected area becomes glassy or tight.
Can Paronychia Infections Recur?
Whether or not a paronychia infection comes back depends on various factors. In cases where antibiotics or antifungal medications don’t completely clear the bacteria or fungus, recurring infections are possible. Additionally, individuals who are prone to chronic paronychia may experience multiple infections.
Taking the appropriate preventative measures and following your physician’s treatment recommendations may greatly reduce the chance of re-infection. If you’ve recently received paronychia treatment and are concerned about lingering or recurring symptoms, be sure to consult with your physician as soon as possible.
Paronychia Risk Factors
While anyone can develop a paronychia nail infection, certain individuals may be at a higher risk. Specific risk factors for paronychia include chronic nail biting, a tendency to develop ingrown fingernails or toenails, and thumb sucking.
Individuals with diabetes mellitus are prone to nerve damage, which can prevent them from physically feeling pain and swelling associated with nail infections, particularly in the toenails. If a person with diabetes is unaware of a worsening nail infection, it can lead to serious complications in some cases.
People with jobs requiring them to immerse their hands or feet in water for extended periods are also at higher risk of developing dry, cracked skin and subsequent nail infections.
Outlook Following Paronychia Treatment
Paronychia nail infections often clear up following treatment, and the overall outlook for recovery is good, especially in mild cases treated with topical medications and/or home remedies. However, it’s imperative to follow your physician’s orders about your specific treatment regimen.
If your physician performed a drainage procedure, the infected area might take a few weeks to heal completely. For individuals treated with surgical procedures to remove the infected nail, it may take several months for the nail to grow back.