Medical professionals will attest to the importance of sleep. However, in reality, Americans just aren’t getting enough. Shocking statistics from the National Institutes of Health note that between 50 and 70 million Americans suffer from sleep issues or a diagnosed chronic sleep disorder. That might mean you aren’t getting the recommended 7 to 9 hours shuteye per night, or it may be that although you leave time to sleep, your quality of sleep is disturbed and/or lacking due to a variety of factors (i.e., sleep apnea, partner snores, diet, or another underlying health issue, etc.).
Here’s what you can expect from a sleep clinic…
1. What Causes Sleep Deprivation?
We can all deal with a few nights, or even a week, or poor quality sleep. However, when sleep deprivation becomes chronic, it can domino affect into a series of unrelated health issues.
For instance, lack of quality shuteye over the long term can lower the immune system’s defences again illness, cause fatigue and interfere with work, cause irritability and other emotional health issues (i.e., depression), and even leave you prone to bad-decisions and injury. If lack of sleep is beginning to impair your quality of life, talking to your doctor about a sleep clinic may be in order.
2. What is a Sleep Specialist?
A referral to a sleep clinic is typically prompted by a visit to your doctor. Your primary care physician can diagnose your symptoms, and if they suspect a sleep disorder (i.e., sleep apnea, insomnia, etc.), may make a referral to a sleep specialist for further diagnosis.
Sleep specialists focus on the diagnoses, evaluation, and treatment of sleep disorders. They can observe you in a sleep clinic setting (either in a hospital or an independent clinic) and pinpoint exactly what’s messing with your quality of sleep.
3. What Qualifies Patients for a Sleep Clinic?
According to research from the National Sleep Foundation, your referral to a sleep clinic will depend on many factors. Your primary care physician will typically refer you based on a series of sleep-related issues, such as your difficulty falling or remaining asleep through the night, as well as your energy levels (or lack thereof) the next morning (i.e., if you suffer from chronic fatigue or impaired function due to lack of sleep).
Your doctor will also inquire about any sleep common sleep disturbances, such as snoring or restless leg syndrome (i.e., itchy, tingling, painful sensations in the legs). Your doctor may ask your spouse or partner if you suffer from sleep apnea, which causes patients to stop breathing momentarily and gasp for air during sleep.
4. What to Expect at a Sleep Clinic
Overnight sleep clinics (or polysomnography studies) are typically conducted either at a hospital or private clinic. However, it’s important that the clinic be accredited by the American Academy of Sleep Medicine.
The experience is non-intrusive, but sets up patients to sleep in their own private, dark, quiet rooms. The patient is typically monitored by video (to observe movement during sleep) as well as audio, as well as wired sensors attached to the legs, chest, scalp, finger, and temples to monitor breathing, heart rate, oxygen blood level, and brain waves during sleep.
5. What to Bring to a Sleep Clinic
Sleep technologists want to mimic your typical bedtime and sleep routine as much as possible in order to get a realistic idea of how you sleep. Other than the wired sensors (which can be a little uncomfortable), you will sleep in a quite, dark, private room (with a bathroom) to ensure the best sleep experience possible.
Patients involved in sleep studies should bring any items they use at bedtime (i.e., special pillows, toothbrush, pyjamas, etc.) to keep the experience as true to your nightly routine as possible.
6. Sleep Disorder Treatment
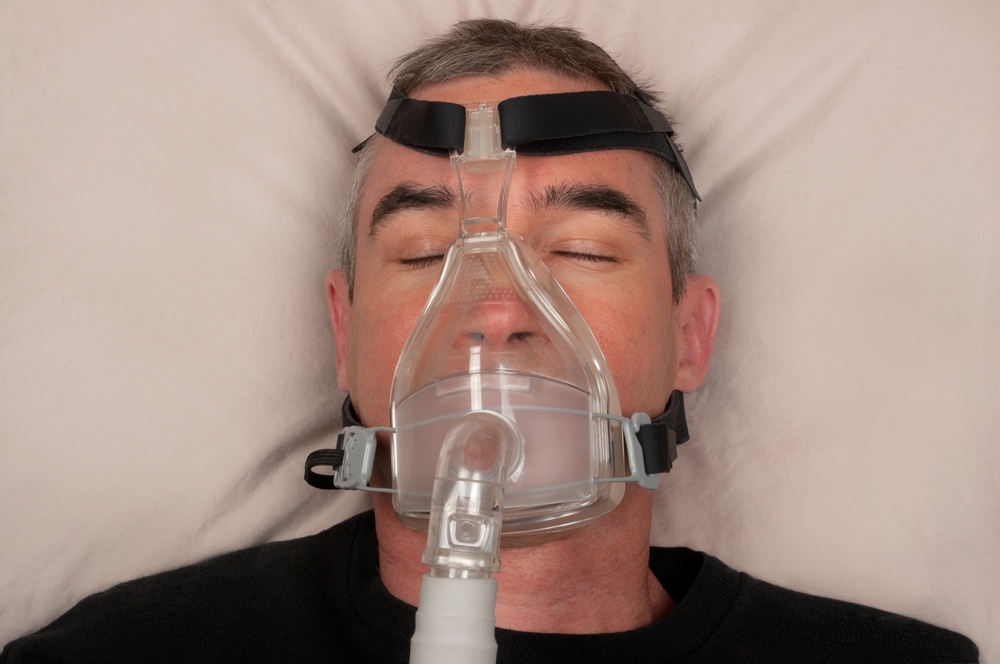
Your night at the sleep clinic will be enough to diagnose the presence of a sleep condition, and possible treatment options. If you suffer from chronic snoring, the sleep specialist may prescribe dental appliances to reduce snoring. In cases where the sleep specialist (or your doctor) thinks a patient may suffer from sleep apnea, you may be asked to sleep wearing a PAP (positive airway pressure) machine.
Further treatment options may include prescription medication (i.e, benzodiazepines such as Klonopin, Valium, and Xanax and non-benzodiazepine hypnotics like Ambien, Lunestra, and Sonata) or cognitive behavioural therapy (for insomnia), in addition to lifestyle tweaks to improve sleep (i.e., reducing caffeine or alcohol, diet and exercise, or adopting a bedtime ritual).