Thanks to the emergence of the “Movember” campaign, awareness of prostate cancer—including how to identify and treat it—has been growing. But we’re far from a cure for this very dangerous disease, which continues to take thousands of American lives each year.
The good news is that breakthroughs are constantly being made in the fight against prostate cancer. From prevention to diagnosis and treatment, medical professionals are working hard to help men prevent, survive and recover from the disease…
Preventive Measures
The fight against prostate cancer starts with prevention. That means examining how lifestyle choices—including diet, exercise and stress—can affect one’s chances of developing this terrible disease. For those involved in this research, the question is this: can exercise or eating certain foods raise or lower one’s risk of getting prostate cancer?
Today, medical experts are making headway in answering these questions. They’ve found that foods high in lycopenes (i.e., tomatoes) and isoflavones (i.e., soybeans) could play an important role in preventing the development of prostate cancer. At the same time, research from the National Cancer Foundation finds that men with high levels of vitamin D, which can be acquired through exposure to sunlight, have a lower risk of developing the more dangerous forms of prostate cancer.
Genetic Research
Genetics plays a major role in determining a man’s risk of developing prostate cancer. Knowing your family history can help medical professionals determine the chances one will have abnormal prostate genes and which drugs to use in order to treat prostate cancer.
Today, medical experts are making important breakthroughs in examining various gene mutations and how this can impact the development of prostate cancer. In some cases, research has shown that certain variants of mitochodrial DNA can significantly raise a man’s chances of developing prostate cancer. As studies continue, this could play a huge role in helping medical professionals identify those men most at risk.
Early Detection
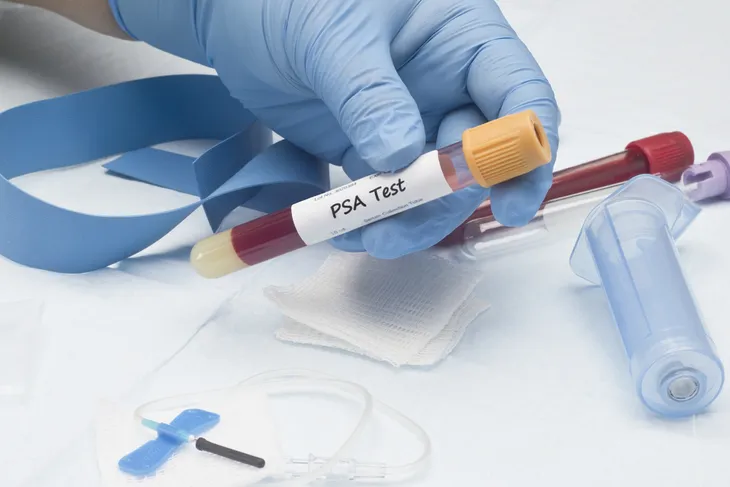
For years, there’s been one major problem with identifying prostate cancer: one of the most popular tests, the prostate-specific antigen (or PSA) blood test, is anything but flawless in detecting prostate cancer before it becomes a significant health threat to the patient. For example, the PSA may miss some threats and point to others that pose no demonstrative risk to the patient.
That’s why medical experts are constantly searching for breakthroughs in detecting prostate cancer. An emerging alternative to the PSA is the “phi,” which blends several test results to develop a clearer picture of a man’s need for prostate cancer treatment. Then there’s the digital rectal exam, or DRE, which can actually push prostate cells into the urine—that means a relatively straightforward urine test can help physicians see if prostate cancer is present.
Diagnostic Measures
For quite a while now physicians have relied on transrectal ultrasound, or TRUS, for carrying out prostate biopsies. However, TRUS, which creates black and white images using sound waves, can miss some areas of the prostate that may contain cancer. Obviously, that’s a big problem for those waging the fight against prostate cancer.
Thankfully, physicians are making significant breakthroughs in making accurate diagnosis of prostate cancer. Perhaps the most important leap forward is a test that measures blood flow within the patient’s prostate gland using color Doppler ultrasound. This can significantly improve the accuracy of biopsies and help doctors detect all cancer threats.
Tracking Development
Once an accurate prostate cancer diagnosis is made, doctors are tasked with carefully tracking the development of the threat. In the past, medical experts have relied on CT and MRI scans for this, but these types of scans are incapable of showing how all of the areas affected by cancer. In fact, it’s particularly difficult for CT and MRI scans to detect how prostate cancer is impacting the lymph nodes.
That’s why medical experts are currently testing a new method known as multiparametric MRI, which is not only more accurate in finding cancer, but can be helpful in showing its aggressiveness. Although it’s far from perfect, this could represent a major breakthrough in the fight against prostate cancer.
Radiation Treatments
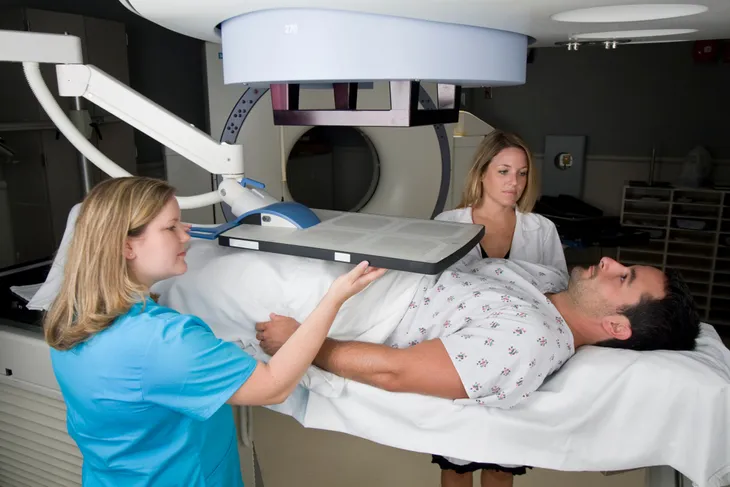
For years, one of the most aggressive ways to treat cancer has been radiation therapy. Unfortunately, this type of treatment can leave the patient sick and exhausted, making it virtually impossible for them to carry out their typical day-to-day activities.
That’s why experts are working on new radiation treatment options that aim radiation far more precisely, thereby limiting a patient’s exposure to radiation. Some methods currently being enhanced including conformal radiation therapy (CRT), intensity modulated radiation therapy (IMRT), and proton beam radiation. The end goal, as you’d expect: beating the cancer without killing off healthy cells and leaving the patient feeling like they’re the ones who’ve taken a walloping.
Hormone Therapy
Hormone therapy represents a world of potential for doctors and scientists involved in the prolonged fight against prostate cancer. The problem is that some forms of hormone therapy have stopped being useful in recent years.
Now, medical experts are focusing on 5-alpha reductase inhibitors—including finasteride and dutasteride—which have the potential to halt the conversion of testosterone to the sometimes problematic dihydrotestosterone (or DHT). Examinations of these drugs are ongoing.