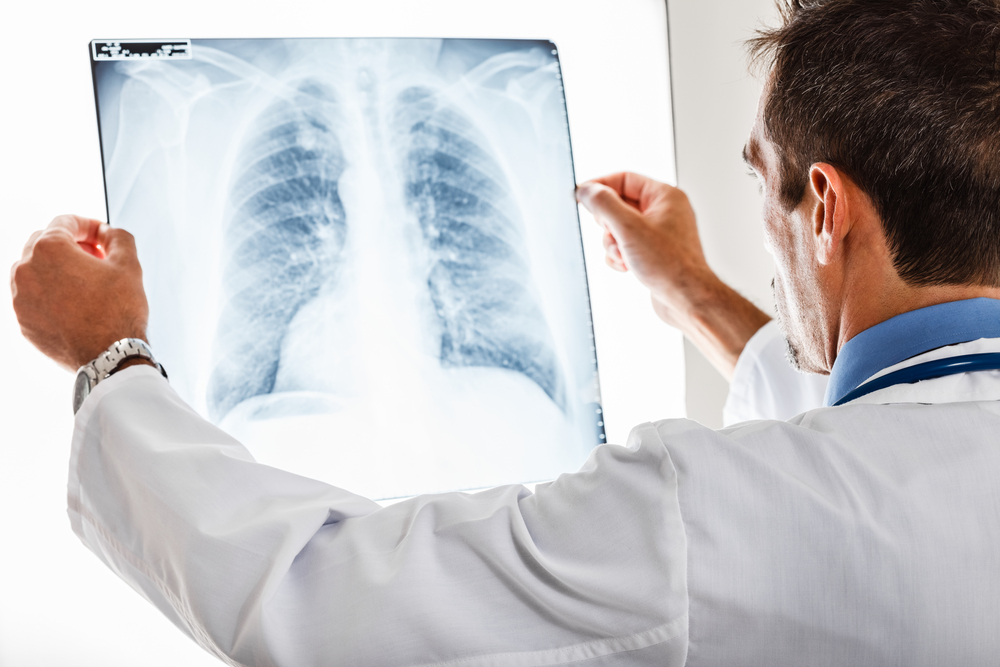
Anyone trying to determine just how seriously smoking can impact your life needs look no further than COPD and its devastating effects. Chronic obstructive pulmonary disease (COPD) is a long-term lung disease often caused by smoking. It includes chronic bronchitis and emphysema, and many people with COPD have both diseases. Imagine trying to breathe when your airways are swollen and blocked by mucus, and the tiny air sacs at the tip of your airways are damaged. With COPD, you are always short of breath and frequently wheezing and coughing, and your cough often produces phlegm. Breathing is also difficult for everyone with COPD, though patient breathing abilities vary greatly and some need oxygen just to walk across the room. To improve breathing, people with COPD are encouraged to stop smoking, they also often participate in pulmonary rehabilitation, and exercise is recommended to whatever extent possible.
Here’s a list of ten things you can do to help offset the effects of COPD…
1. No More Smoking
Sure it’s possible to contract COPD through long-term exposure to environmental pollutants, but smoking is the primary cause of COPD. Once you have it your lungs are already damaged, so the key becomes reducing future harm. According to one expert, sufferers should stop smoking immediately when they become short-winded. Neil MacIntyre, MD, a pulmonologist and professor of medicine at Duke University Medical Center in Durham, North Carolina, stresses this to his patients. He adds that “if you want to get out of a hole, the first thing you must do is stop digging”.
2. Avoid Bad Air
In many large metropolitan areas there is an industrial section where the air is polluted and less than ideal for breathing. People with COPD are advised to stay away from any such area because the resulting toxins may exacerbate their lung problems. Similarly, they should also be watchful for others things in their environment that may cause flare-ups and breathing difficulty—such as construction sites; places where there is second-hand smoke or fumes of any kind; and environments where there may be high amounts of pollen, dust and even perfumes. At home, using air filters can help, as can turning on the air conditioner where allergens are problematic.
3. The All-Important Medication
While there is no cure for COPD, the taking of prescribed medications can help lessen its symptoms. Taking the correct medicine can allow someone with the disease to be more active, have less coughing and shortness of breath, and get fewer flare-ups. It’s important for the patient to take a leading role in their treatment. This means knowing which medicine they are taking and how and when to take them, and understanding who to speak with if there are any questions or problems. Regular visits with a family doctor or specialist will help keep the medications current and address any changes in symptoms or affect.
4. Pulmonary Rehab
Think of pulmonary rehabilitation as ongoing treatment for those with serious lung problems. It is strongly recommended for people with COPD and can teach them how to breathe easier, live better, and conserve energy in day-to-day activities. An emphasis is placed on breathing techniques and getting the most out of each breath. Patients are also taught how to exercise properly without overdoing it and are often given the chance to practice these exercises in a group setting. Exercises may include walking on a treadmill and the light lifting of weights. Therapists will also give their patients breathing tips; for instance, don’t bend over when lifting things to keep from compressing the lungs.
5. The Weight Issue
Achieving the correct weight is enough of a problem for most people. When you have COPD, it becomes an even greater issue. Those very sick with the disease use a great amount of energy to breathe and have problems keeping on the pounds and maintaining a healthy weight. They often need to eat more to gain weight. Meanwhile those that are overweight are faced with the predicament of trying to shed pounds to improve their breathing. It may be helpful to seek the input of a physician, specialist, and a nutritionist to achieve an ongoing balance of nutritional needs and maintaining a safe weight.
6. Stay Healthy
The advice makes so much sense that it’s nearly redundant. Of course we should stay healthy. But for a person living with COPD this piece of guidance has deeper implications. With their compromised lungs, they can have an awful time getting rid of an infection. Plus, common colds or the flu can sometimes transform into pneumonia, more easily than it can for people without COPD. It is recommended that COPD patients avoid people that are sick and big crowds. They should call their physician in the early stages of a cold or flu, and get an annual flu shot and pneumonia vaccination roughly every five years.
7. Seek Easy Sleep
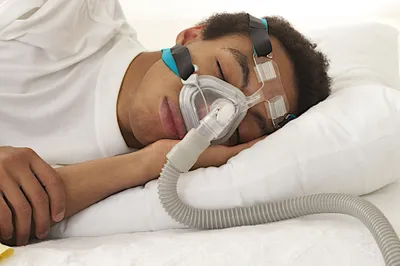
When we begin to feel ill, many of us live by the mantra “it’s nothing that a good sleep won’t cure.” That advice won’t help many people with COPD. They often have sleep disorders—such as sleep apnea or hypoventilation (breathing that is too slow or shallow)—and experience symptoms such as feeling tired and falling asleep during the day, morning headaches and excessive snoring. Their route to sleep may come through the use of a mask for continuous positive airway pressure (CPAP) therapy. A CPAP machine isn’t the most convenient way to sleep (think of wearing a gas mask that’s attached to an air pump machine) but for many it’s the only way to get good sleep, and a far better alternative than hardly any sleep.
8. Get Active
It’s not just a universal message; for people with COPD it could be one of the most important things they do on a daily basis to cope with their disease. Daily movement won’t directly change the level of lung functioning, but it can improve cardiac function and muscle tone. Exercise allows for an easier delivery of oxygen to the muscles and increases stamina. COPD patients need to be careful to not push their limits to the point where they can’t breathe. Walking a couple of blocks may be enough for some. Rest in between periods of walking can help. Eventually, the person may walk longer distances without shortness of breath.
9. Breathe In, Breathe Out
Breath is of the essence for people with COPD and ideally they learn to inhale and exhale as well as possible, early on in their disease. In COPD rehab, two primary exercises are practised to help cope with the effects of limited breath. The first is pursed-lip breathing, which helps solve the problem of air getting built up in the lungs. It also aids with shortness of breath. To do this, inhale deeply through the nose, and then purse lips as though whistling, and breathe out three times more slowly than breathing in without forcing the air out. The second exercise is diaphragm breathing, which aids in strengthening the diaphragm muscles so you use less energy when breathing. Here’s how it works: lie on your back with your knees bent, one hand on your upper chest and another resting on your abdomen. When you inhale and exhale, keep your chest as still as possible and use your stomach to breathe. Do this for 5 to 10 minutes three times daily.
10. Lung Transplant Surgery
There are two main types of procedures performed on people with COPD. The first is a lung transplant. Raed Dweik, MD, director of the pulmonary vascular program at Cleveland Clinic notes this is only an option for certain people with COPD because there is a “transplant window—you can’t be too sick, but you have to be sick enough.” There are major risks involved with lung transplants, the first and foremost being moderate survival rates: an estimated 78-percent the first year after surgery, 63-percent after three years, and 51-percent five years out (according to the U.S. National Heart, Lung, and Blood Institute). Also, anti-rejection medicine can suppress the immune system for the rest of the person’s life. But, for some patients the quality of life they stand to gain makes for an easy decision. The second type of procedure is volume reduction surgery where the damaged lung tissue is removed to make the lungs work more efficiently.