Your doctor told you that you need a colonoscopy. Now what? The procedure might sound frightening and we bet you have lots of questions. No need to stress, we’re here to cover how often you should have a colonoscopy and everything you need to know –the before, during, after, and everything in between. We promise it isn’t as scary as it sounds!
A colonoscopy is a procedure doctors use to take a look at the inside of your intestine and colon. They will be able to see any changes that may need special attention. There is a special prep that you will need to follow the day before the procedure. During the colonoscopy, you will be asleep. Once the procedure is over you’ll wake up and be on your way out the door.
But that’s not it, there’s a lot more to a colonoscopy and that’s what we’ll talk about below, so keep reading.
Why Do I Need a Colonoscopy?
A colonoscopy is performed for several reasons. The main reason is as a screening tool for colorectal cancer. The doctor can look for signs of cancer or signals of a precancerous growth like a polyp. According to Healthline, “The American College of Surgeons estimates that 90-percent of polyps or tumors can be detected through colonoscopy screenings.” The CDC recommends that adults over 50 years and under 75 years be screened for colorectal cancer.
Colorectal cancer isn’t the only reason your doctor may order a colonoscopy. The procedure can look for causes of unexplained abdominal pain, bleeding, weight loss, or changes in your bowel habits. If your doctor suspects you have conditions like Crohn’s disease or ulcerative colitis you will likely need a colonoscopy for a diagnosis. If your doctor requests that you get a colonoscopy make sure you understand why you need it.
Diet Changes For a Colonoscopy
The week before your colonoscopy you will need to make some diet changes. Your doctor will give you specific instructions on what you need to do but in most cases, you will need to avoid eating:
- Seeds and nuts
- Raw vegetables
- Whole pieces of corn kernels
- Whole grains (ie oatmeal and brown rice)
In the 24 hours leading up to your procedure, your doctor will likely ask you to avoid eating solid foods. You can drink clear liquids which include water, coffee, sports drinks, and apple juice. WebMD does say that you’ll need to stay away from anything red, blue, or purple. The dyes in these drinks can temporarily change the color of the inside of your intestine.
About 3 to 4 hours before your actual colonoscopy your doctor will instruct you to not eat or drink anything (medically known as NPO, nothing by mouth). Always check with your doctor on their specific instructions regarding the timing for your diet changes.
Medications
If you regularly take medications then you might need to adjust or stop it before your colonoscopy. If you do not receive specific instructions on which medications can be continued and which need to be stopped call your doctor. Each person and situation is different. These are the most common medications that need to be stopped or adjusted:
- Medication that regulates glucose in the blood
- Diuretics
- Blood thinners
- Nonsteroidal anti-inflammatory drugs (NSAIDs)
The Real Preparation
So now you know everything about what you can and cannot eat before your colonoscopy. It’s time to cover the “actual” prep that your doctor will order. Each facility or doctor will have their own specific instructions but they will generally look like this. The night before your colonoscopy your doctor will have you take a stool softener and laxative. The stool softener will get your bowels prepped for the laxative.
The laxative part is what most people least enjoy. The most common medication doctors order is the laxative polyethylene glycol (MiraLAX). It draws fluid into your intestine making your bowel movements more liquidy. In the case of a colonoscopy prep, you will be ordered to take a large amount of polyethylene glycol and continue to take it until your stool is water-like. You’ll want to stay close to the bathroom during this part because you’ll be visiting it often.
Pre-procedure Check In
It’s the day of your colonoscopy and you’re packed up and ready to go. But wait, make sure you have someone to drive you to and from from your procedure. You will be sedated for your colonoscopy and most centers won’t even start the procedure if they have not confirmed you have a driver home. Once you’ve gotten your drive squared away and are all checked in a nurse or medical assistant will escort you into the pre-procedure room.
This is the room where you’ll have your vital signs checked and health history reviewed. The gastroenterologist who is performing the procedure may stop by and ask a few questions as well. They will want to make sure the night before prep went well and that you were able to clean out your intestine for the colonoscopy. If you did not complete the prep they may have you reschedule the procedure. After all of this is done then it’s time for the actual procedure.
The Actual Procedure
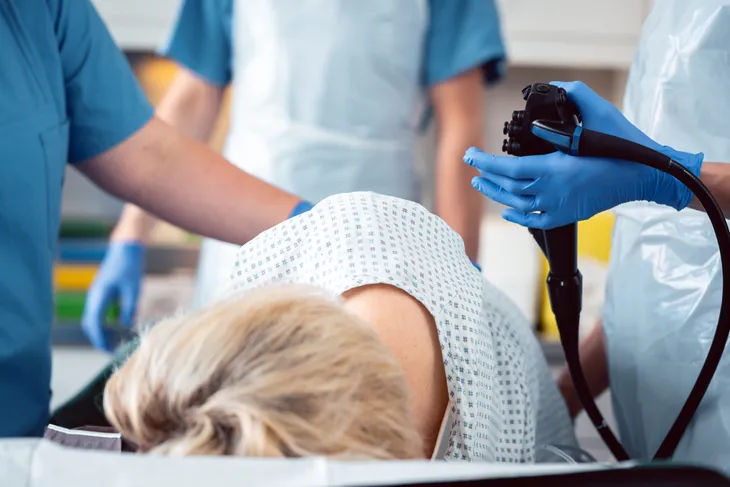
The question and answer session is done and it’s time to get the show on the road! You will be brought into the colonoscopy procedure room (sometimes the pre-procedure room is the room where the colonoscopy happens). The gastroenterologist and nurse will position you onto your left side. Medication will be administered through an IV to make you fall asleep.
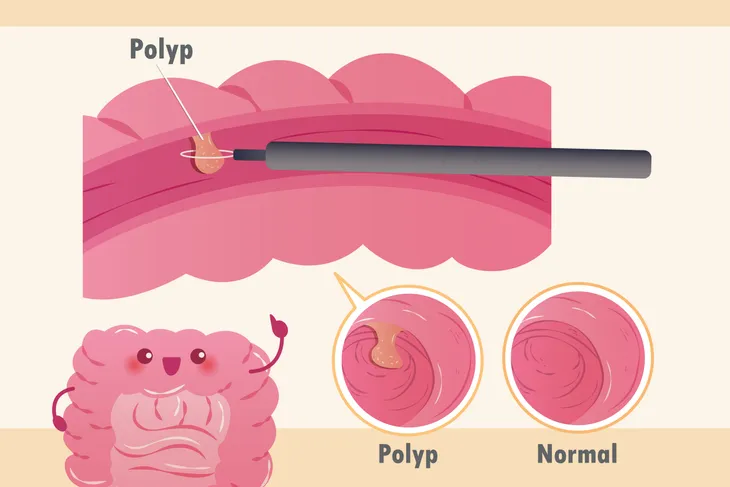
As you sleep a small tube called the colonoscope will be placed into your rectum. The scope is small in diameter (only a half inch) but long enough to thread through your intestine. There is a camera at the end of the scope that relays images to a screen in the procedure room. This allows the gastroenterologist to see your intestinal walls and look for problem areas. If your doctor finds polyps they may remove them during the procedure. The whole colonoscopy will take anywhere from 20 to 30 minutes.
Recovery
After the colonoscopy is complete you will wake up. Your abdomen might feel distended from air being pumped into your intestine during the procedure. You’ll feel groggy and have a hard time keeping your eyes open at first. But slowly you’ll wake up and feel back to normal. A nurse or doctor might tell you what was seen during the colonoscopy but often times you’ll need to wait for an official report from your doctor’s office.
Once you are awake enough you can eat and drink whatever you like. Take is slow though, some people can feel nauseous after sedation. After you’ve been discharged your designated driver can take you back home to rest and recuperate.
Your Results
As you wait in the recovery area after your colonoscopy your doctor might come by and talk to you about their findings. They might look over images from the colonoscopy and any follow-up tests that might be necessary. “However, there might be a wait of several days before the results of the colon biopsy are available. The doctor should be able to advise the person about how long they might have to wait” reports Medical News Today.
If your doctor does find polyps or precancerous cells then you may need to have more frequent colonoscopies or possibly surgery. Always be sure to ask your doctor to clarify any test results that you do not understand and have a clear idea of the next steps that need to be taken.
When To Call Your Doctor
Once you’ve settled in at home after your colonoscopy you may notice that your stomach is bloated or that you have a little bit of blood in your stool. These are normal findings after a colonoscopy but if it continues for days after there may be a problem that needs to be addressed by your doctor says Healthline.
Make sure to look over your discharge instructions that were given to you before you left the procedure facility. This handout should list who and when to call if certain scenarios should arise. Call your doctor if you have abdominal pain, a fever, or have bowel movements that contain blood clots or blood.
Colonoscopy Risks
A colonoscopy is a very common procedure done all over the country more times than we could possible know. In almost every case, the benefits of finding cancer, precancerous cells, or polyps far outweigh the risk of the procedure. But that doesn’t mean the procedure doesn’t come without any risk at all.
The potential risks of having a colonoscopy are tearing the intestinal wall, bleeding, and adverse reactions to the sedation. Before you have your procedure your doctor should cover all the potential complications and have you sign a waiver acknowledging these risks. If you do not completely understand the risks ask questions for clarification.
When Will I Need Another Colonoscopy?
No one wants to go through the prep of a colonoscopy and thankfully most people will only need to have the procedure done once every 10 years. “People older than 75 should talk with their health care provider about if they should keep getting screened,” says the American Cancer Society. If something was found during your colonoscopy then you will likely have to have another one sooner, your doctor will let you know.
Colonoscopies are a common screening procedure that can detect cancer or precancerous lesions. The prep may be unpleasant but the test can save lives. Always follow your doctor recommendations on when you should have a colonoscopy. The best case is that they find nothing and you won’t need to have another one for 10 years. But if your doctor does find polyps or cancer then the colonoscopy may have just saved your life.