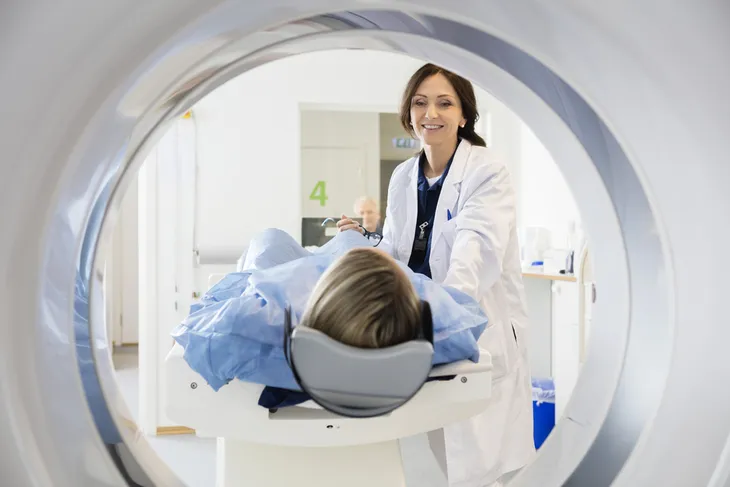
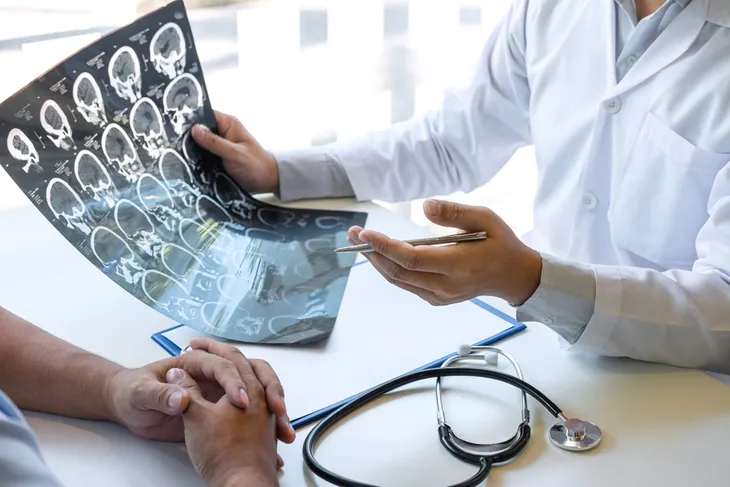
- Cerebral cavernous malformations (CCMs) are irregular bundles of tiny blood vessels in the brain.
- Although this condition is rare, it can be life-threatening and may lead to long-lasting health problems.
- It’s primarily a genetic condition and may be treated with medication. In serious cases, surgery may be necessary.
Cerebral cavernous malformations, also known as CCMs, are abnormally formed blood vessels. While this might give you pause for concern, it is rare, occurring in 0.2-percent of the general population. However, in severe cases, this condition can be life-threatening and may lead to long-lasting health problems, which is why it’s important to get informed.
But first, we should explain what this condition means, and who it affects. That way, you will have a better understanding of the condition and visit a doctor if you have concerns (or call 911 for serious complications). Here’s everything you need to know about cerebral cavernous malformations…
What Are Cerebral Cavernous Malformations?
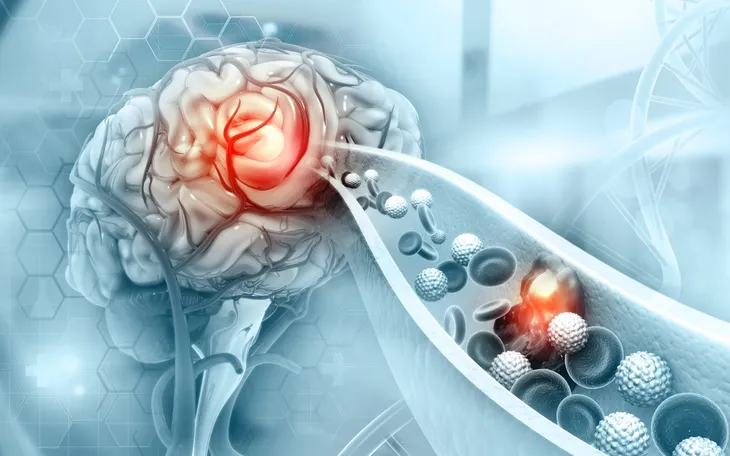
As WebMD puts it, CCMs are “irregular bundles of tiny blood vessels (capillaries) in the brain.” More specifically, it notes that the vessels are stretched out more than the norm, which leads to their walls being prone to leaking.
The CCMs can range in size from about a 1/4-inch to 4-inches, says the source. It also explains that the vessel walls “also lack certain fibers that normally make blood vessels able to stretch out and then stretch back,” causing their shape to change with high blood flow. The vessels then end up in “odd open spaces” referred to as caverns.
 novak.elcic / Shutterstock
novak.elcic / ShutterstockWhat Causes CCMs?
First off, the National Library of Medicine explains that the condition affects up to 50-people per 10,000 globally (it’s considered fairly rare). CCMs are primarily a genetic condition — specifically, the mutation of three or more genes: KRIT1, CCM2, and PDCD10, notes the source. “Mutations in these three genes account for 85 to 95 percent of all cases of familial cerebral cavernous malformations,” it claims.
However, the source also notes that there are two forms of this condition — familial (FCCM that’s more prevalent among Hispanic populations) and sporadic. The former is passed down from a parent and can cause several CCMs. The latter develops in patients that have no family history of the condition and may be less severe.
CCMs Usually Present in Adulthood
The American Heart Association (AHA) Journals explains that the “mean age of presentation” for vascular malformations associated with CCMs is about 37-years. However, that doesn’t mean younger or older people can’t show signs of the condition — although the source says the prevalence of CCM associated with developmental venous anomalies (DVA) grows with age.
However, the same source explains that about 25-percent of CCM cases occur within the pediatric population, “with most of the literature from this age group generally reporting on particular location as brain stem, spinal cord, and basal ganglia.”
There Can Be Unusual Developmental Signs
WebMD says there are some “less commonly” recognized symptoms of CCMs. They include “unusual muscle growth,” as well as an abnormal skin texture or skin growth, explains the source. These are in addition to the blood flow issues associated with CCMs, which can be identified using medical techniques, which we’ll explain in more detail later.
In children, it can be difficult to recognize the signs of a CCM, says C.S. Mott Children’s Hospital, the University of Michigan Health. “Additionally, it can also be difficult to determine what are normal developmental issues, and what could be related to a change in a CCM,” it says. Contact a pediatrician if you have concerns about recent changes in your child.
They Can Cause Vision Issues
As we mentioned before, sometimes those who are shown to have CCMs will have no related symptoms. However, the Mayo Clinic explains that vision issues can occur from “recurrent episodes of bleeding or blood clot formation.”
More specifically, it says that it can cause “focal” or vision issues that include a loss of vision or double vision. There can also be balance problems associated. If you notice some unexplained changes in your sight, then it’s always wise to consult a physician or optometrist.
CCMs Can Lead to Cognitive Decline
Johns Hopkins Medicine explains that CCMs can affect the brain in a variety of ways. For example, patients sometimes have “difficulty thinking clearly or with remembering things,” which could also be a sign of other conditions such as dementia.
It also notes that most patients that display symptoms (including this one) are between 20 and 50-years of age. It may be difficult to gauge a younger child based on their memory or ability to communicate.
Neurological Problems May Occur
The Mayo Clinic says the “most concerning complications” of this condition is progressive neurological damage as a result of multiple hemorrhages. This can affect a person’s ability to function normally in their day-to-day life. (Possible outcomes include paralysis or loss of sensation in parts of the body).
The hemorrhaging is considered a complication of CCMs and is more likely in patients who have experienced prior hemorrhaging. Those with malformations centered in the brainstem are also more at risk of this complication.
 DimaBerlin / Shutterstock
DimaBerlin / ShutterstockSeizures Are Common
Johns Hopkins Medicine explains that headaches and seizures among patients are common, depending on where the “lesions” are located, and how abundant they are. Most symptoms occur in people that have CCMs in the brain or spinal cord.
A seizure is a reason to seek emergency medical help through calling 911 or visiting an emergency room. Keep in mind, a seizure may not be a result of a CCM as there are different types of seizures with varying symptoms. Nonetheless, they are a cause for concern and need to be addressed by a medical professional.
 Shutterstock/ldutko
Shutterstock/ldutkoStrokes Are Another Serious Complication
Aside from seizures, CCMs can also lead to serious strokes. In severe cases, they can be fatal. The National Institute of Neurological Disorders and Stroke says these cavernous malformations, when located in the brain and spinal cord, can cause “hemorrhagic strokes” — that’s another way of saying bleeding in the brain.
This type of stroke usually occurs when an artery in the brain is leaking or bursts, which can cause brain cell damage from the pressure. There are other risk factors for strokes, ranging from high blood pressure to alcohol abuse to genetic causes.
When to Visit a Doctor
We already noted that a seizure is a definite reason to get medical help — and fast. But there are other reasons to pick up the phone to a healthcare provider, explains Johns Hopkins Medicine.
Among these other triggers are “severe” headaches (vomiting from the headache is another warning sign), as well as feelings of numbness in the body or physical weakness. It’s also wise to recognize the signs of a stroke to seek help fast in an attempt to limit the damage.
How Are CCMs Diagnosed?
A doctor will likely take a medical history and administer a physical exam to narrow down suspicions of CCMs. From there, a doctor can confirm a CCM through the use of medical imaging that detects abnormal blood flow.
These imaging methods include magnetic resonance imaging (MRI), computed tomography (CT) scan, as well as an electroencephalogram that detects electrical activity in the brain. Additionally, some clinics may use blood tests and genetic testing to get a proper diagnosis.
How Are CCMs Treated?
WebMD says that doctors may opt to treat only the symptoms of the CCMs, rather than the vascular abnormalities themselves. One approach is to prescribe anti-seizure medication if that’s a complication, explains the source. Doctors can also turn to pain medications or refer patients to rehabilitation exercises if there’s mobility loss.
In some serious cases, the medical team may opt for more serious measures. That could include surgery if medications aren’t working and if CCMs have clearly been identified as the cause of your health issues. The team will weigh the benefits of surgery against the risks.
Many Cases Aren’t Extreme
The good news, explains WebMD, is that many people won’t even know they’re dealing with a CCM. Others have some mild symptoms that can be managed with the right medications and proper rest.
However, as previously noted, sometimes there are “life-changing” complications related to CCMs that can be permanent. So far scientists haven’t found an effective way to prevent CCMs, but genetic research may change this in the future.