- Central sleep apnea is a disorder in which your breathing stops and starts during sleep.
- Though both obstructive sleep apnea and central sleep apnea involve abnormal breathing patterns during sleep, they are different.
- Left untreated, it can lead to serious health consequences so it’s important to know the signs and seek medical attention if they develop.
Are you feeling extremely tired during the day? Perhaps you wake up with morning headaches or have unexplained shortness of breath. These could all be key warning signs that you’re suffering from central sleep apnea.
Central sleep apnea is typically caused by an underlying health condition and if left untreated, it can lead to serious health consequences. So it’s important to get informed. Here’s what you need to know about central sleep apnea, including what it is, how it differs from obstructive sleep apnea, and the common causes. We’ll also find out how it’s diagnosed and the potential treatment options.
What Is Central Sleep Apnea?
Central sleep apnea is a disorder that causes you to briefly stop breathing when sleeping. You may experience moments of apnea repeatedly throughout the night. But why can this happen?
According to WebMD, your breathing may be interrupted if your brain has a problem with signaling. When this happens, the brain doesn’t send “proper signals to the muscles that control your breathing.” explains the source.
Obstructive Sleep Apnea vs. Central Sleep Apnea: What Is the Difference?
Both obstructive sleep apnea and central sleep apnea involve abnormal breathing during sleep. But what sets them apart is their causes.
According to the Sleep Foundation, in obstructive sleep apnea, “a person makes a notable effort to breathe, but the airway is blocked.” Central sleep apnea, on the other hand, is not caused by a blocked airway. It results from a signaling problem with the brain and the muscles that control breathing.
Central sleep apnea is also far less common than obstructive sleep apnea, accounting for only about 20-percent of all sleep apnea cases.
Common Symptoms of Central Sleep Apnea
Unfortunately, the Sleep Foundation says many people don’t experience symptoms. Often, they find out they have the condition after visiting the doctor for another reason. However, when symptoms do occur, they’re usually associated with “fragmented sleep and abnormal levels of oxygen in the blood,” says the source.
Some symptoms that may indicate you’re suffering from central sleep apnea include insomnia or chest discomfort at night. If you wake up with shortness of breath, this can also indicate central sleep apnea, as can excessive tiredness during the day, difficulty concentrating, and headaches in the morning.
The Warning Signs of Central Sleep Apnea
The Sleep Foundation says since central sleep apnea often doesn’t cause noticeable symptoms there are a few warning signs you should look out for that may indicate your breathing is interrupted during sleep. The first warning sign is unexplained excessive daytime sleepiness. When your sleep is interrupted repeatedly throughout the night, you can be left feeling extremely tired during the day. Some people may even be so tired they fall asleep during the day.
Another warning sign of central sleep apnea is poor sleep. Feeling tired even after a long night of rest can be a sign that your sleep is poor. If you suddenly develop insomnia, this can also be a warning sign of central sleep apnea. If you share a bed or have a caregiver, the source also suggests asking them to observe your sleep. They may be able to notice other warning signs like abnormal breathing patterns.
What Causes Central Sleep Apnea?
We already know that central sleep apnea occurs when your brain doesn’t send proper signals to the muscles that control your breathing but what causes your brain to have a problem with signaling? Healthline says it’s usually caused by an underlying health condition that affects your brain stem, spinal cord, or heart.
Possible conditions that can cause central sleep apnea include stroke, heart attack, and congestive heart failure. Inflammation in the brain (encephalitis), arthritis in the cervical spine, and a weak breathing pattern (Cheyne Stokes breathing) can also cause central sleep apnea. The source also notes that Parkinson’s disease, surgery or radiation treatment to the spine, as well as some medications, may also be the culprit.
Who’s At Risk?
Certain factors may increase your risk of central sleep apnea, such as your age. The Sleep Foundation says central sleep apnea is more common in people over 65-years.
Central sleep apnea is also more common in males. The source says it might be due to “the effects of testosterone on the amount of carbon dioxide that can accumulate in the blood before the body reflexively takes a breath.” Certain medications may also increase your risk.
Since the disorder is typically caused by an underlying medical condition, having any of them can also increase your risk. If you’re worried about your risk of central sleep apnea or are showing signs of the disorder, contact your doctor right away.
How Is Central Sleep Apnea Diagnosed?
If your doctor suspects central sleep apnea, they’ll start by reviewing your medical history and current symptoms. Your doctor will also likely do a physical exam to try and rule out other causes.
To confirm a diagnosis, doctors typically order a sleep study test, known as a polysomnography. The Sleep Foundation says the test takes place at a sleep laboratory which is usually in a hospital or sleep center.
What to Expect During a Sleep Study
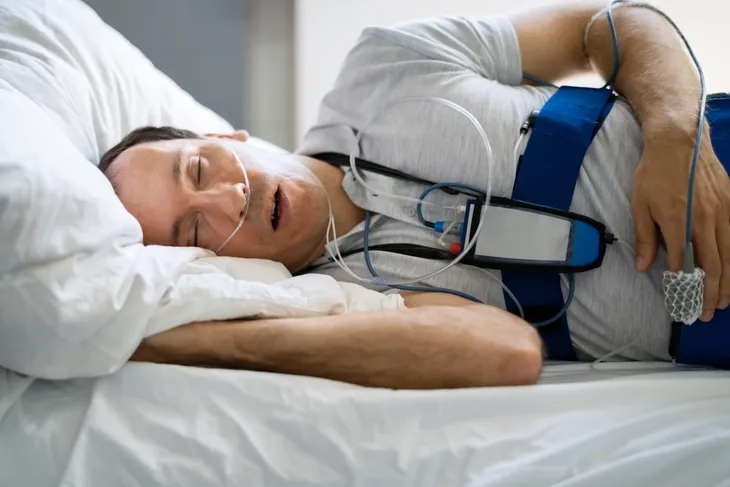
Preparing for any medical test can be nerve-wracking, especially when it’s your first time but rest assured, a sleep study is noninvasive. Ahead of the test, you’ll meet with a medical professional who will explain the entire process and what you can expect, as well as the steps you’ll need to take to prepare.
The sleep test takes place overnight, which means you’ll sleep at the sleep center. A medical professional will hook up electrodes to your head and body, which measure your brain activity, breathing patterns, oxygen levels, heart rate, and lung function. You’ll be monitored during the test and then your results will be reviewed.
How Is Central Sleep Apnea Treated?
If central sleep apnea is diagnosed, your medical team will devise a treatment plan. The goal of treatment is to help your breathing patterns during sleep return to normal, which in turn can improve your quality of sleep and reduce your daytime symptoms.
Since central sleep apnea is typically caused by an underlying health condition, treatment will be aimed to help resolve the underlying cause. Treatment may also involve positive air pressure (PAP) therapy, adaptive servo-ventilation (ASV), supplemental oxygen, medication, or nerve stimulation. Let’s take a closer look at what these involve next.
Treatment: Positive Airway Pressure (PAP) Therapy
One treatment option is positive air pressure (PAP) therapy. This treatment uses a special machine that helps you breathe during sleep by pumping air into your airways. There are a few different types of PAP machines including continuous airway pressure (CPAP), bilevel positive airway pressure (BiPAP), and adaptive servo-ventilation (ASV).
Both CPAP and BiPAP devices involve wearing a face mask while you sleep. Healthline says that CPAP provides a steady source of pressure in your airways whereas Bipap adjusts the air pressure to a higher level when you inhale and a lower level when you exhale.
If a CPAP doesn’t effectively treat your disorder then ASV may be recommended. ASV delivers air pressure dynamically and adjusts the pressure based on your breathing patterns.
Treatment: Supplemental Oxygen
Another treatment option is supplemental oxygen. This involves a device that provides your lungs with extra oxygen during sleep.
Sometimes it’s recommended in conjunction with PAP therapy, while other times it’s recommended if PAP therapy isn’t working. Your doctor will determine which option is best for you.
Other Treatment Options
In some cases, medication may be necessary. The Sleep Foundation says the goal of medication is to stimulate breathing. However, they often have side effects, so you’ll have to be monitored by your doctor when taking them.
If other treatments fail to resolve the disorder then phrenic nerve stimulation may be necessary. This option is invasive and involves “surgically implanting a device in the chest that encourages breathing,” explains the source. Once the device is implanted, it can send an electrical current to the nerve to make the diaphragm contract, which returns your breathing to normal.
Tips for Living With Central Sleep Apnea
Some people require daily treatment which can be hard to live with. But the Sleep Foundation outlines a few effective tips to help you cope with the disorder. For starters, the source suggests learning everything you can about the condition. Leaning on support groups can also help you feel less alone.
It’s also important to identify any triggers that may cause an episode of abnormal breathing. If you know what they are, do what you can to avoid them. Finally, the source also says it’s important to regularly visit the doctor. Follow-up visits are important to ensure your current treatment is working and to address any complications or side effects.