Borderline personality disorder (BPD) is a mental illness that affects about 1.6-percent of adults in the United States alone. According to the National Health Services (NHS), it is the most commonly recognized personality disorder and affects a person’s thoughts and feelings about themselves and others.
Those who develop BPD tend to begin exhibiting signs by early adulthood. The condition generally worsens as they move into young adulthood, but it can get better as they age. Read on to learn the most common symptoms and biggest risk factors of BPD to be mindful of.
Symptoms
Fear of Abandonment
People with BPD tend to have a strong fear of being left alone or abandoned. Regardless of whether such abandonment is real or imagined, the individual may go to extreme measures to avoid possible separation or rejection.
For example, HelpGuides.com says someone with BPD may “beg, cling, start fights, jealously track your loved one’s movements, or even physically block the other person from leaving.” Unfortunately, these behaviors may cause loved ones to withdraw, resulting in exactly what they feared and were trying to prevent.
Unstable Relationships
BPD tends to make maintaining healthy relationships very challenging. This is because the affected individual tends to be quite needy, intense, and mistrusting, not only with romantic partners, but also with friends and family.
Additionally, a person with BPD tends to have a very black and white way of thinking about people, seeing them as “all good” or “all bad.” This causes frequently shifting attitudes towards others that range from “extreme closeness and love (idealization) to extreme dislike or anger (devaluation),” says the National Institute of Mental Health.
 Shutterstock/fizkes
Shutterstock/fizkesUnstable Self-Image
People with BPD also struggle with identity disturbances. Sometimes, they may feel good about themselves, but other times they may feel hatred toward who they are, perhaps seeing themselves as bad or evil. Additionally, this self-image can change depending on whom the person is with, as they often copy the actions and behaviors of others. “Their ability to be independent and autonomous is very impaired,” says John Oldham, MD, professor of Psychiatry and Behavioral Sciences at Baylor College of Medicine in Houston, in speaking with Health.com.
They may also have constantly shifting ideas of who they are or what they want in life, resulting in frequent changes to “jobs, friends, lovers, religion, values, goals, and even sexual identity,” indicates HelpGuides.com.
Impulsive, Risky Behaviors
Impulsive, risky, and often self-destructive behaviors are also common for those with BPD. These behaviors can include gambling, spending sprees, shoplifting, or “sabotaging success by suddenly quitting a good job or ending a positive relationship,” says the Mayo Clinic.
In some cases these behaviors may even put the individual in danger, such as by driving recklessly, practicing unsafe sex, abusing drugs or alcohol, or binge eating. While engaging in these activities may help them feel better in the moment, they can do more harm than good to themselves and their close relationships in the long run.
Self-Harm
Self-injury is another common symptom of BPD; in fact, the Centre for Addiction and Mental Health says that “up to 75 percent of people with BPD self-injure one or more times,” commonly by cutting, burning themselves with cigarettes, or an “overdose that can bring relief from intense emotional pain.”
While in most cases these self-harming behaviors are parasuicidal, that isn’t the case for everyone, as the source reports, “about 10-percent of people with BPD take their own lives.”
Suicidal Thoughts
While in most cases these self-harming behaviors are non-suicidal, that isn’t the case for everyone, as the source reports, “about 10 percent of people with BPD take their own lives.” Suicidal thoughts and behavior are not uncommon for those who struggle with BPD. This suicidal behavior includes thinking about suicide, making suicidal threats, or actually carrying out a suicide attempt.
Intense Mood Swings
Another common symptom of BPD is emotional volatility, with intense mood swings that range from extreme happiness one moment to despair the next. These mood swings can be triggered by things that others would simply brush off or not even notice, such as “if a colleague was too preoccupied to say hello in the hallway” says Health.com.
While these mood swings tend to pass fairly quickly, typically lasting only a few minutes or hours, they may persist for several days at a time in some cases.
Chronic Feelings of Emptiness
People with BPD may also struggle with chronic feelings of emptiness, as if “there’s a hole or a void inside them,” says HelpGuides.com. In extreme cases, the source says that individuals may feel as if they are “nothing” or “nobody.”
Because this feeling of emptiness is uncomfortable, they “may try to fill the hole with things like drugs, food, or sex.” While these things may offer temporary relief, nothing seems to make it go away for good.
Explosive Anger
In addition to extreme mood swings, people with BPD may also struggle with intense anger. Although such anger is often triggered, Health.com says they “react in a way that seems exaggerated or disproportional to an event.”
These reactions can include “frequently losing your temper, being sarcastic or bitter, or having physical fights,” says the Mayo Clinic. Although this anger is most noticeable when it is directed outwardly toward others, HelpGuides.com notes that people with BPD spend a great deal of time being angry at themselves.
Paranoia
Paranoia is another common symptom of BPD, where an individual may have “suspicious thoughts about others’ motives,” says HelpGuides.com. As a result, they may struggle to trust others. Episodes of paranoid thinking or paranoia can range from mild and temporary to severe and chronic depending on the person.
Dissociation
In some cases, often when under stress, people with BPD may experience dissociation or a feeling of losing touch with reality. In such a state, the National Institute of Mental Health says they may “feel cut off from oneself, seeing oneself from outside one’s body, or feelings of unreality.”
Anxiety
Those with borderline personality disorder may also struggle with bouts of anxiety or chronic anxiety. They may experience intense episodes of anxiety, fear, or worry which can last from a few hours to a few days or sometimes longer. An anxiety disorder can be a separate diagnosis altogether, but it often does come as a symptom or side effect alongside BPD.
Depression
Another common sign or symptom of BPD is feelings of depression, hopelessness, or low energy. These feelings are more than just normal sadness and are typically more chronic or intense in nature. Depression is another symptom that can be diagnosed as its own disorder but often does come as a common sign or symptom alongside BPD.
Difficulty Feeling Empathy
Those with borderline personality disorder often have a difficult time feeling empathy for others. Studies have shown that those with BPD often have reduced activity in the brain regions that support empathy which can lead to difficulty maintaining interpersonal relationships. This reduced activity means that those with BPD have a hard time understanding and predicting how others may feel in certain situations.
Unstable Plans And Aspirations
Another indicator of BPD is a feeling of instability towards career plans, aspirations, and goals. Those with BPD may lack the motivation or energy to bring their plans to life or feel scatter-brained while making these plans. BPD causes frequent changes in likes and dislikes which often makes it difficult for those who have been diagnosed to commit to one career path. BPD patients may also struggle with an unstable self-image which makes it challenging to grow in a career.
Risk Factors
Genetics
BPD is believed to be caused by a combination of factors, one of which is genetics. If someone in your close family, such as a parent or sibling, has also been diagnosed with the mental illness, the NHS says the genes you inherit “may make you more vulnerable to developing BPD.”
But, so far, there’s no evidence of a BPD gene. Mind.org.uk says “Genetics might make you more vulnerable to developing BPD, but often it’s due to stressful or traumatic life experiences that these vulnerabilities are triggered and become a problem.”
Childhood Distress
What types of stressful or traumatic life events might trigger these genetic vulnerabilities? A few that are noted by the U.S. National Library of Medicine include “either real or fear of abandonment in childhood or adolescence,” a “disrupted family life,” or “poor communication in the family.” The NHS adds that experiencing chronic fear or distress during childhood may also contribute.
Childhood Abuse
Another factor that may contribute to BPD is “sexual, physical or emotional” abuse from childhood. There is evidence that those diagnosed with BPD are more likely to have had a history of abuse or other distressing experiences during childhood. Studies have shown that “40% to 76% of people with BPD report that they were sexually abused as children, and 25% to 73% report that they were physically abused.”
Childhood Neglect
Another form of childhood abuse that can be more passive but just as impactful is childhood neglect which can be both physical and emotional. Examples of physical neglect include denying a child basic necessities such as food or water. Emotional neglect is when a child’s basic emotional or mental needs are ignored.
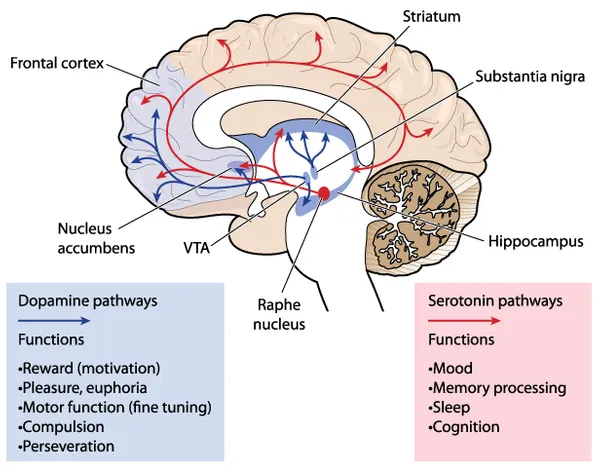
Serotonin Abnormalities
Another factor that is believed to contribute to BPD is abnormalities with neurotransmitters—chemicals that transmit signals between cells in the brain. One neurotransmitter that is of particular concern is serotonin.
According to Healthline.com, “Serotonin is a hormone that helps regulate mood,” and improper amounts of it cause noticeable changes. These changes can include “depression, aggression and difficulty controlling destructive urges,” notes the NHS.