- More than 1 million Americans suffer from shingles each year.
- Shingles can sometimes be hard to identify because it often mimics other conditions such as poison ivy or scabies.
- Some telling signs of shingles include blisters, itching, headache, fever, chills, and extreme fatigue.
- If you suspect you have shingles, contact your doctor right away.
Each year more than 1 million Americans suffer from shingles, an itchy, blistering rash caused by herpes zoster, which is the same viral infection that afflicts the nerve roots and causes chickenpox. In fact, those who’ve had chickenpox can end up with shingles years later (often after the age of 50) due to the fact that the infection lives dormant in the body. It can become active and again with age, lowered immunity, a medical treatment (i.e., radiation) or medication that suppresses immunity, or an infection (i.e., HIV).
The issue with shingles is that it often mimics other conditions, such as poison ivy or scabies, with similar uncomfortable symptoms. However, there are a few telling signs that give shingles away, including…
Want senior content delivered straight to your inbox? Sign up for our exclusive email list and receive articles and news on diet & nutrition, fitness, and mental health dedicated specifically to our senior audience!
Rash
When the shingles virus activates, it causes a rash that has painful, fluid-filled blisters, which often appear on one side or area of the body. This happens because the virus affects localized nerve roots, typically in the chest, back, buttocks, or neck, and remains directly connected to those exact areas for about 7 to 10 days. Initially, the blisters will be filled with a clear fluid, but after a few days, the fluid will cloud up and take on a darker, murkier hue.
Most patients report feeling generally unwell in the days leading up to the rash, with some saying they developed a mild form of the flu. These flu-like symptoms are usually accompanied with swollen lymph nodes, which may be tender to the touch.
Tingling Sensations
Tingling sensations are often reported alongside flu-like symptoms that precede the outbreak of a shingles rash. These tingling sensations usually manifest as extreme sensitivity to touch in a localized area of the body or on one side of the body. Patients also report itching, burning, and numbness, which is usually contained to the areas of the body where the rash later appears.
Doctors believe that these tingling sensations occur because the virus that causes shingles affects nerve roots. Thus, the nerves in affected areas respond to a stimulus that is only present on a microbial level. You’ll experience sensitivity, tingling, itching, and burning for no apparent reason. The most common sites of these tingling sensations include the back, chest, abdomen, face, neck, head, or one arm or leg. It almost never affects both sides of the body simultaneously.
Nausea
Nausea can occur leading up to the shingles rash. You might first dismiss this symptom as being something mundane, but it’ll quickly progress into more flu-like symptoms. In most cases, patients report a general feeling of nausea or queasiness, which may worsen when in certain body positions. Some people experience diarrhea and/or vomiting. However, vomiting is relatively rare.
One of the definitive aspects of the nausea and flu-like symptoms that precede a shingles outbreak is that they are not typically accompanied by a rise in body temperature. You may feel fevered even though the body temperature is still in a normal range.
Stomach Pain
Alongside the nausea, patients may also experience stomach pain ahead of a shingles outbreak. In most cases, the stomach discomfort is relatively mild. However, it’s still noticeable enough to raise some alarms that something is wrong. Sharp stomach pain could be a sign of shingles if it occurs alongside other flu-like symptoms.
Headache
The shingles virus will often cause neuropathic pain in the cranial nerves and nerve roots, which will result in a painful, recurring headache that often won’t be alleviated by over-the-counter (OTC) headache medications. This is because the headache is being triggered by interference with your nerves, a condition that most OTC pain relievers aren’t designed to deal with.
Fever
Earlier, we mentioned that the flu-like symptoms seen in shingles cases won’t normally cause a rise in body temperature. However, this isn’t a hard-and-fast rule that applies to every case. In some rare cases, patients may develop a fever. It doesn’t happen often, but when it does, it can be serious. It is not uncommon for shingles fevers to exceed 101-degrees Fahrenheit (38.3-degrees Celsius).
The best treatment for fever is bed rest and plenty of fluids. However, if the fever is accompanied by additional symptoms, such as a stiff neck, breathing problems, or a severe headache — go to a doctor. Any fever above 102-degrees Fahrenheit should be seen by a doctor. The same is true of fevers that last for more than a few days, and of fevers that become increasingly severe over the course of a continuous 24-hour period.
Chills
Experiencing chills is very common before the shingles rash breaks out, due to fluctuations in body temperature and the immune system’s natural response to a viral infection. These chills are not usually localized, but rather, seem to affect the entire body. This often misleads patients into thinking they have nothing more than the regular flu, when in fact, they are experiencing the early symptoms of a case of shingles.
As with many other shingles symptoms, chills can only be managed through palliative treatment designed to improve the patient’s overall level of comfort. Listen to your body and respond accordingly. If you’re feeling cold, warm up by putting on extra clothing or staying under a blanket. If you’re too warm, cool down by removing clothing or adjusting the indoor temperature. Unfortunately, chills can be difficult to manage because patients tend to swing back and forth between feeling hot and cold. In such cases, keep as comfortable as possible, avoid strenuous activity, and drink plenty of fluids.
Eye Issues
Vision complications can occur if the shingles virus spreads to nerves that connect to the eyes. This will cause eye pain in bright environments, a condition known as “photosensitivity.” In extreme cases, a nasty eye infection (called “conjunctivitis” or “pink eye”) can occur. Conjunctivitis can cause inflammation and the development of a gooey, sticky sticky coating on the eyelashes. Treatment options include the introduction of artificial tears to keep the eye moist, and cold packs to help moderate the temperature of surrounding tissues.
These symptoms should be considered very serious. If you develop them, seek immediate medical attention. Untreated eye-based symptoms caused by shingles can lead to temporary or permanent vision impairment, even blindness. While these outcomes are rare, they are present nonetheless; permanent damage usually results from complications arising from excessive dryness in the eye or poorly regulated temperature of the nearby tissues.
Muscle Pain
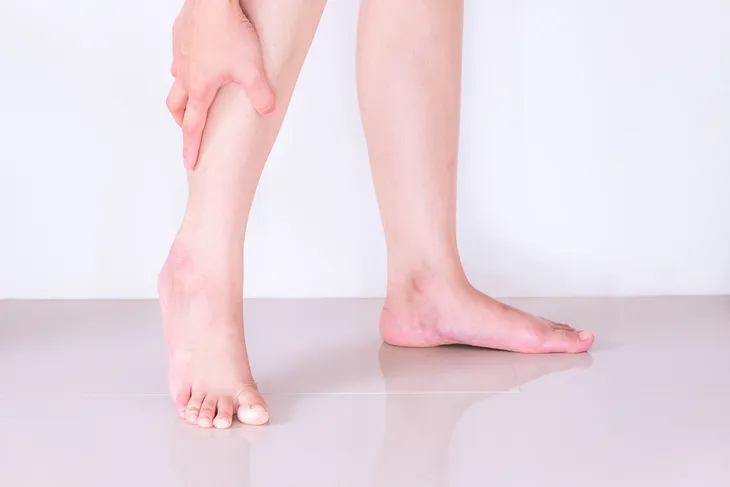
Muscle pain (or “myalgia”) is often an early warning sign of shingles. This usually presents as a particularly painful tingling or a feeling of “piercing needles” in the skin, and it most often occurs in the muscles of the arms and legs. Alternately, patients may experience sensations of tenderness or soreness in muscles that have not been overworked, along with other symptoms of malaise.
Like headaches, this type of muscle pain can linger for extended periods of time, even after the case of shingles has died down. This lingering muscle pain is part of the postherpetic neuralgia syndrome, and it can be very difficult to treat. Rarely, it lasts for very long periods of time; some patients claim it affects them for many years afterwards. However, like postherpetic neuralgia headaches, lingering muscle pain usually goes away on its own within 30 days.
Extreme Fatigue
Most individuals who’ve had shingles will complain, in the days preceding its full-on outbreak, of lethargy or a feeling of being completely drained of energy for no apparent reason. This can lead to longer periods spent sleeping, or overwhelming urges to take daytime naps. Despite the patient’s best efforts, attempts to increase energy levels are usually only met with temporary results. Many people increase their caffeine intake, which leads to more frequent urination, causing dehydration and an intensification of the malaise and fatigue symptoms.
In some cases, patients may experience confusion or even memory loss for no apparent reason. Thankfully, most patients go on to recover fully from these symptoms once shingles is resolved. It is extremely uncommon for any such problems to linger for weeks or months after other symptoms have gone away.
Sensitivity to Touch
Extreme sensitivity to touch is often a complaint of shingles patients. This sensitivity commonly affects the forehead and chest, causing eating, sleeping, and daily activities to be very uncomfortable or almost impossible. In almost all cases, this sensitivity is most pronounced in areas with that telltale shingles rash.
This sensitivity to touch usually presents itself before the rash breaks out, with patients reporting that certain localized parts of their body suddenly feeling tender, painful, or highly reactive to even light external stimuli. As a result, sleeping can be difficult as bedsheets and certain bodily positions put pressure on these areas. Sensitivity symptoms usually peak within a few days to a week after the rash appears before subsiding as the patient’s condition improves. However, they can linger as part of the postherpetic neuralgia syndrome experienced by a minority of people who have otherwise fully recovered.
 Shutterstock/goodluz
Shutterstock/goodluzPostherpetic Neuralgia
Unfortunately, a significant number of people who develop shingles will continue to experience pain and headaches even after the disease has run its course. In extreme cases, this lingering discomfort can last for months or even years.
The condition is known as “postherpetic neuralgia.” It is often concentrated in the forehead when it affects the head region. In a best-case scenario, postherpetic neuralgia will resolve itself within about 30 days. You may require additional care and specialized treatment afterwards to help with lingering symptoms.
 Shidlovski / Shutterstock
Shidlovski / ShutterstockItching
Before the shingles rash appears, people will often experience itchiness. The itchiness occurs where the rash develops. This can happen anywhere from days to weeks before the rash appears. The sensation can vary, meaning it can come and go. There may also be burning or tingling and often accompanied by other symptoms.
Cause of Shingles
Shingles is a viral infection which means it’s caused by a virus. The name of the virus is the varicella-zoster virus which also causes chickenpox. People who have already had chickenpox can develop shingles as it reactivates the virus in their body, explains Healthline.
Unfortunately, still to this day health experts aren’t sure why some people get shingles and others don’t. However it does seem to be more common in older adults who have lower immunity to infections. Healthline provides a list of other risk factors for shingles which includes a weak immune system, emotional stress, aging adults, and someone undergoing cancer treatments or a major surgery.
Complication: Long-Term Nerve Pain
Some people may develop long term nerve damage due to shingles. This long lasting pain could be a symptom of postherpetic neuralgia. This pain could last up to the first year to 18-months after shingles goes away. Patients must learn how to manage their pain until it subsidies, or until a doctor recommends a treatment.
Complication: Ramsay Hunt Syndrome
Anyone with shingles symptoms on or around the ears should seek treatment immediately. This can lead to Ramsay Hunt syndrome if left untreated. Symptoms of this illness include dizziness, earaches, hearing loss, and ringing in your ear.
Some people may even experience a loss of ability to move parts of your face. The good news is this complication is rare, as long as people receive early treatment for their shingles.
Complication: Swelling
Another severe complication that can develop from shingles is swelling or inflammation in the lungs, brain, or liver. This is a life threatening complication that is uncommon, but something to still look out for. Seeing your doctor regularly during a shingles outbreak can help ensure your condition does not reach this level of danger.
Other Possible Complications
There are some other complications you may experience long-term with shingles. In fact, up to 4-percent of people with shingles get hospitalized for complications. Some complications like long-term nerve pain and swelling are more dangerous than others, but there are less severe complications too.
For instance, shingles is a rash that has blisters break open and crust over. It’s important for you to keep these clean and dry to lower the risk of developing a bacterial infection. This effect also makes it more likely that your skin will have scarring.
Risk Factors of Shingles
Anyone who has had wild-type varicella zoster virus (VZV), also known as chickenpox, is at risk of developing shingles. This also applies to those who’ve had the varicella vaccination. Your increase for hospitalization due to shingles rises after the age of 50. It’s also highly contagious, so be aware if you’ve interacted with anyone that may have shingles.
Those living with certain conditions that compromise their immune system gave an increased risk of getting shingles. This includes cancer, human immunodeficiency virus (HIV), bone marrow or solid organ transplant recipient, and anyone taking immunosuppressive medications.
Prevention Tips
According to the National Institute on Aging (NIA), the best form of prevention is the shingles vaccine, also known as varicella-zoster immunization. This is available for adults who are 50 and older. While it can’t stop it completely, it prevent severe symptoms and complications.
Children should get the chickenpox vaccine, also known as varicella immunization. Adults who never had the chickenpox should also get this vaccine. Again, it doesn’t mean a child or adult won’t ever get chicken pox, but Healthline points out the success rate is high. It can prevent it in 9 out of 10 people.
Treatment Options
There is no immediate cure for shingles. The best thing form of treatment is to minimize the severity of symptoms. The Centers for Disease Control and Prevention (CDC) says there are several antiviral medicines available that can help treat shingles and shorten the duration of the illness. The most common are acyclovir, valacyclovir, and famciclovir. If you suspect you have shingles, contact your doctor right away. They will be able to provide a diagnosis and move forward with treatment.
In addition to the antiviral medication, there is also pain medicine, either OTC or prescribed by a doctor. These will help provide relief from the pain associated with shingles. The CDC also recommends using wet compresses, calamine lotion, and a colloidal oatmeal bath. These may help relieve any itchy symptoms.
When to See a Doctor
If you’re experiencing pain and rash near the eyes, you should see a doctor immediately. Don’t wait for the rash to spread further around the body because this can lead to extreme complications. Those over the age of 60 or have a weakened immune system should not wait to see their doctor if experiencing any symptoms.
 Vitalii Vodolazskyi / Shuttertstock
Vitalii Vodolazskyi / Shuttertstock