There’s no denying that being diagnosed with ovarian cancer — or any form of cancer, for that matter — can be very scary. The good news is that there are a number of treatment options available to patients based on how early the cancer was detected.
In terms of how invasive these treatment options are, they range from taking medications to complex surgical procedures. Typically, if the cancer is detected early, it will be treated with less invasive options first before proceeding to surgery, if it’s determined to be necessary at all.
Other factors to consider when determining the most appropriate treatment option for a patient include age and overall state of health. With that in mind, let’s take a look at several prominent treatment options a patient can consider along with physicians and other medical professionals.
Natural/Alternative Medicine
There are many cancer patients who find the average clinical environment cold, threatening, even dangerous. Others seek alternatives to prescribed medications that can come with many side effects — like drowsiness, fatigue and vomiting — that make taking them hugely difficult. In search of something else, many cancer patients reach out to naturopaths and others who consider themselves specialists in alternative health treatments.
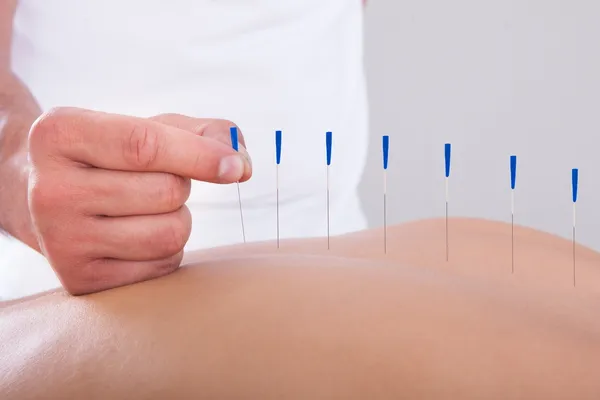
Alternative medicine is actually a massive field, with treatments ranging from simple teas and tonics to taking otherworldly plant-based medications. Other alternative treatments may be designed to simply help a cancer patient manage their diagnosis — take, for example, massage or acupuncture. Still other alternative treatments can help by making small or more significant changes to a patient’s diet. Of course, a patient being treated for ovarian cancer should discuss these alternative treatments with their doctor before proceeding.
Support Groups
The world’s best cancer specialists understand that treating a serious form of cancer, like ovarian cancer, requires a holistic approach. That means not only treating the body by targeting the cancer and trying to remove it, but helping the patient handle the mental hurdles that come with a cancer fight.
Many cancer specialists and cancer-focused clinics can help patients find support groups made up of people facing similarly intense and intimidating health challenges. Although discussing an ovarian cancer diagnosis with a support group won’t cure the cancer, it can help a patient see that they’re not the only ones waging such a difficult fight. In doing so, it can provide the patient with the mental strength they need to win such a fight.
Ovarian Cancer Surgery
Surgery to remove any form of cancer, particularly ovarian cancer, tends to be highly complicated and requires a long recovery time. However, this is the standard of treatment for ovarian cancer. This is considered “debulking” and decreases the tumor load so chemotherapy can be more effective. While the surgery may be complicated, it can now be done robotically which decreases the recovery time. In many ovarian cancer cases there’s simply no choice: without surgery, the patient increases their risk of dying.
Surgery for ovarian cancer will vary in style, nature and intensity based on several factors, including the patient’s age, the extent of the cancer, and the patient’s overall health. Surgical procedures for ovarian cancer can be limited, such as removing a small tumor from the body, or more complex and invasive, such as removing the entire ovaries or even uterus. To determine the best course of action, a family doctor will refer the patient to a gynecologic oncologist, a specialist with training in all facets of ovarian cancer, including surgery.
Chemotherapy for Ovarian Cancer
Following a diagnosis of ovarian cancer, many physicians recommend their patient undergo chemotherapy, which involves using a series of potent medications to restrict the cancer’s growth and spread. Chemotherapy is often used in cases where the ovarian cancer has metastasized, or expanded to other parts of the body. These powerful drugs have the potential to limit this growth, giving physicians more time to devise an effective strategy for removing the cancer. Sometimes chemotherapy is used prior to surgery to try to decrease the size of the tumor before surgery, but more commonly, chemotherapy is used after surgery.
Women diagnosed with ovarian cancer may receive their chemotherapy drugs through injection into a vein or have them taken orally, like most other drugs. However, in some cases of ovarian cancer, physicians will recommend injecting chemotherapy drugs directly into the abdominal cavity through the use of a catheter. Widely known as intraperitoneal chemotherapy, this method can allow for the chemotherapy drugs to enter the bloodstream and spread throughout the body quicker.
Targeted Therapy
Targeted therapy is, in some ways, like chemotherapy. Both involve the use of potent drugs to stop or limit the spread of cancer cells. However, unlike chemotherapy, which typically involves spreading drugs throughout the entire body, targeted therapy is just as it sounds — it targets a specific part of the body most affected by cancer cells, rather than the whole human form.
The advantage of treating ovarian cancer this way is obvious: it can significantly reduce the number of side effects and complications related to the drugs being taken. Targeted therapy depends on the use of drugs that can effectively identify, attack, and divide cancer cells, preventing them from repairing themselves or spreading further. Unfortunately, targeted therapy remains an emerging strategy and may not be applicable in all cases of ovarian cancer.
Hormone Therapy
The use of hormones or drugs capable of effectively blocking hormones can be effective in the fight against ovarian cancer. Typically, injections are made every one to three months.
One type of this medication, luteinizing-hormone-releasing hormone (LHRH) agonists, is used to lower estrogen production in women who have not yet reached menopause. This can help to limit the growth of ovarian cancer but does come with some significant side effects, most of which reflect menopause-like symptoms.
Hormone therapy is the use of hormones or hormone-blocking drugs to fight cancer. This type of systemic therapy is rarely used to treat epithelial ovarian cancer, but is more often used to treat ovarian stromal tumors.
Tamoxifen
One of the most prevalent drugs available to breast cancer patients is Tamoxifen, which is also employed in some ovarian cancer cases (it’s effective against some types of ovarian cancer, but not others).
Tamoxifen is most effective in reducing levels of estrogen, which can help to encourage the growth of cancer cells. Unfortunately, by reducing estrogen levels, Tamoxifen can introduce a number of uncomfortable side effects, including hot flashes. One major health problem introduced by the use of Tamoxifen is the increased risk of developing blood clots in the legs.
Aromatase Inhibitors
Aromatase is an enzyme that, in postmenopausal women, can effectively transform hormones into estrogen. Given that estrogen has the potential to stimulate and encourage the growth of cancer cells, the aromatase enzyme can have an adverse effect on efforts to limit the spread of ovarian cancer.
As the name suggests, aromatase inhibitors help to limit the activity of the aromatase enzyme and lower the production of estrogen. Aromatase inhibitors are most popular in the fight against breast cancer, but has been shown to be effective in ovarian cancer cases as well. As with other drugs that impact hormonal production, aromatase inhibitors can lead to several menopause-like side effects, including hot flashes and muscle pain.