Cholesterol is a waxy substance in the blood. Our body needs it to build healthy cells, but too much can increase our risk of heart disease. High cholesterol (hyperlipidemia), is a condition characterized by excessive fats, or lipids, in the blood. There are about 3-million new diagnosis of this condition in the U.S. alone, each year.
The National Cholesterol Education Program (NCEP) recommends all adults 20-years and older be screened for hyperlipidemia at least every five-years. Screening is done with a blood test called a fasting (nothing to eat 8 to 12 hours prior to blood draw) lipid panel. A normal test is total cholesterol <200, LDL (“bad” cholesterol) <160, HDL (“good” cholesterol) >40, and triglycerides <150. To get better informed on high cholesterol, here are 12 ways to help manage it…
1. Diet
High cholesterol has the potential to accelerate atherosclerosis, or hardening of the arteries caused by deposition of fats and cholesterol. A diet with reduced intake of saturated fats, trans fats, and cholesterol is recommended for individuals with hyperlipidemia. This type of diet is often referred to as a “Mediterranean diet.” Olive oil is the staple fat of this diet. A diet of varied, colorful fruits and vegetables and whole grains is also recommended for hyperlipidemia.
Individuals with hyperlipidemia should also increase their intake of fiber, which has the potential to decrease cholesterol levels by as much as 10-percent. Fish, nuts, and beans and other legumes should also be included in the diet. Reduced intake of red meat, processed meats, and fried foods is recommended. Dairy products should be low fat or fat free. For example, skim milk is a better choice than whole milk.
2. Regular Exercise
Regular exercise is recommended for individuals with high cholesterol. It can lower LDL (“bad”) cholesterol and raise HDL (“good”) cholesterol. Regular exercise can also lower total cholesterol and triglyceride levels. It can also help shed extra pounds. Individuals with hyperlipidemia are recommended to exercise for 30-minutes most days of the week. Furthermore, it does not have to be continuous and could be done in 10-minute blocks.
Regular exercise can include activities like walking, swimming, running, weight training, biking/cycling, and dancing. Lack of exercise increases an individual’s risk of heart disease by increasing levels of LDL cholesterol. Regular exercise can have a positive impact on other risk factors for heart disease such as high blood pressure (hypertension), obesity, and diabetes. It is highly recommended that individuals consult with their health care provider before commencing an exercise program.
3. Weight Loss
Being overweight or obese, increases an individual’s chances of developing high cholesterol. High cholesterol, or hyperlipidemia, is a risk factor for the development heart disease. Body mass index (BMI) is an indirect measure of body fat and therefore health. Overweight is defined as a BMI greater than 25, but less than 30. Obese is defined as a BMI greater than 30. In the United States, approximately 75-percent of adults and 30-percent of children and adolescents are considered to be overweight or obese.
Weight loss is the most effective way to lower triglyceride levels. It can also lower total cholesterol and LDL (“bad”) cholesterol, and raise HDL (“good”) cholesterol levels. A weight loss of 10-percent can significantly lower an individual’s risk of developing or reversing high cholesterol. Maintenance of weight loss is best accomplished by a permanent lifestyle change, or else individuals gain back every pound and more.
4. Quit Smoking
Everyone understands that smoking is bad for an individual’s health. Smoking increases an individual’s risk of developing high cholesterol. Specifically, smoking raises LDL (“bad”) cholesterol and triglyceride levels. It can also lower HDL (“good”) cholesterol levels. Smoking damages the walls of arteries making them more susceptible to the accumulation of fat and cholesterol deposit, hardening, and narrowing (atherosclerosis). Atherosclerosis directly contributes to the development of heart disease.
Individuals diagnosed with high cholesterol should quit smoking as soon as possible. The most well documented effect that smoking has on cholesterol is the lowering of HDL (“good”) cholesterol levels. HDL cholesterol actually protects the body against heart disease, and that effect is lost with smoking. An article published September 2013 in the journal Biomarker Research concluded HDL levels could rise by as much as 30-percent within three weeks of quitting smoking. Furthermore, the risk of heart disease drops by as much as 30-percent within a year of quitting smoking.
5. Moderate Alcohol Consumption
Moderate alcohol consumption may increase levels of HDL (“good”) cholesterol in the blood, which decreases the risk of developing heart disease. Unfortunately, it does not lower LDL (“bad”) cholesterol in the blood. Moderate alcohol consumption is defined as one drink a day for females and two drinks per day for males. A drinks is defined as 12-ounces of beer, 5-ounces of wine, 1 ½-ounces of 80-proof liquor, or 1-ounce of 100-proof liquor.
Heavy alcohol consumption can boost levels of triglycerides in the blood. It can also have other negative effects such as high blood pressure (hypertension), anemia, cancer (mouth, throat, voicebox, and esophagus), cardiomyopathy (disease of heart muscle), arrhythmias (abnormal heart rhythms), liver disease, memory loss, pancreatitis (a dangerous condition characterized by inflammation of the pancreas) and heart disease. Heavy alcohol consumption may also decrease the effectiveness of cholesterol-lowering medications such as the statins.
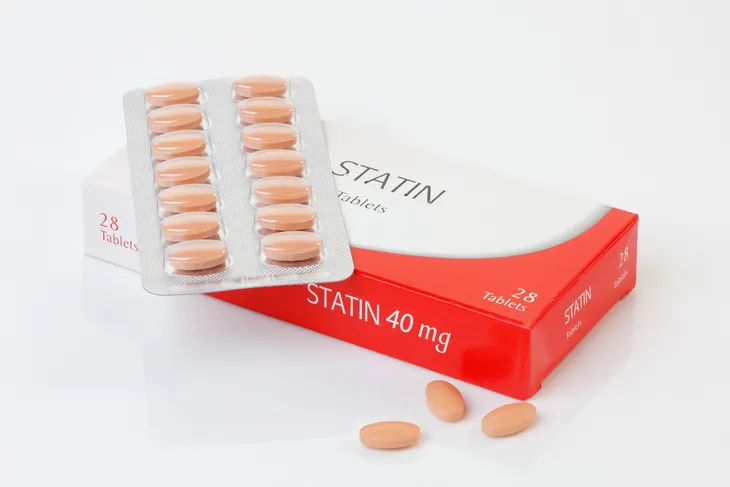
6. Statins
The most commonly prescribed class of medications to treat high cholesterol is the statins. Statins approved by the United States Food and Drug Administration (FDA) include atorvastatin (Lipitor), fluvastatin (Lescol), lovastatin (Mevacor), pravastatin (Pravachol), rosuvastatin (Crestor), and simvastatin (Zocor). They work by blocking an enzyme in the liver responsible for the production of cholesterol. In clinical studies, statins have been shown to reduce the occurrence of heart attacks, strokes, and death in the general population.
With regard to their ability to lower cholesterol, atorvastatin (Lipitor) and rosuvastatin (Crestor) are the strongest, while fluvasatin (Lescol) is the weakest. Statins have numerous interactions with other drugs, which should be reviewed by a physician. The most common side effects of statins may include headache, nausea, vomiting, rash, diarrhea, constipation, weakness, and muscle pain. Statins may cause elevated liver enzymes, but serious liver damage is rare. After statins hit the market, there have been reports of memory impairment.
7. Niacin
Niacin, also known as vitamin B3, has been shown to improve cholesterol by raising HDL (“good”) cholesterol and lowering LDL (“bad”) cholesterol and triglyceride levels. Examples of prescription-strength niacin include Niacor and Niaspan. Individuals should refrain from purchasing niacin over-the-counter (OTC) because the doses aren’t effective. Niacin combined with a statin has the possibility of boosting HDL cholesterol levels by as much as 30-percent. Niacin is the only drug proven to consistently raise HDL cholesterol levels.
One of the most common side effects of niacin is flushing (redness and warmth in the face and neck). Taking aspirin prior to the dose of niacin may reduce flushing. Other side effects may include nausea, vomiting, diarrhea, jaundice (yellowing of the eyes and skin), elevated liver enzymes, ulcers, itching, and tingling in the hands and feet. As a result of side effects, niacin is usually reserved for individuals not tolerating therapy with a statin.
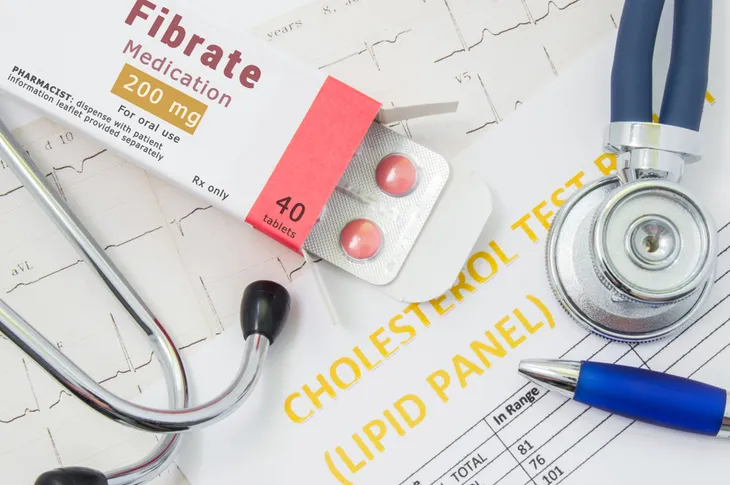
8. Fibrates
Fibrates, also known as fibric acid derivatives, can be used to treat high cholesterol. These drugs primarily lower triglyceride levels and can modestly boost HDL (“good”) cholesterol levels. Of note, fibrates are not effective at lowering LDL (“bad”) cholesterol levels. Examples of prescription fibrates include gemfibrozil (Lopid) and fenofibrate (Tricor). Fibrates can be used alone or with other cholesterol lowering drugs such as statins.
Side effects of fibrates may include diarrhea, gallstones, constipation, inflammation of the liver, dizziness, stomach upset, and dizziness. Individuals with kidney problems, liver disease, or gallbladder disease should refrain from taking fibrates. When taken in combination with statins, fibrates may increase the likelihood of muscle damage.
 Shidlovski / Shutterstock.com
Shidlovski / Shutterstock.com9. Bile Acid Resins
Bile acid resins assist the body in the disposal of LDL (“bad”) cholesterol. Bile is produced in the liver by the breakdown of hemoglobin, a protein in red blood cells. The body uses cholesterol to produce bile, which is released during the digestive process. Resins bind bile and prevent it from being absorbed in the digestive process. The body answers by making more bile, which consumes more cholesterol. As the cycle is repeated, levels of cholesterol in the blood drop.
Three bile acid resins are available in the United States—cholestyramine (Questran), colestipol (Colestid), and colesevelam (Welchol). Resins are the most senior and safest cholesterol lowering drugs. They are less potent than other classes available today such as the statins. Side effects of resins may include constipation, heartburn, nausea, indigestion, and flatulence (gas). Individuals with liver or gallbladder disease should refrain from taking resins. Bile acid resins are usually reserved for individuals not tolerating therapy with a statin.
10. Fish Oil
Fish oil contains omega-3 fatty acids, which may be beneficial in lowering triglyceride blood levels. The omega-3 fatty acids are EPA and DHA. The recommended dose of fish oil is four grams per day. Over-the-counter (OTC) fish oil supplements vary in their concentrations of EPA/DHA. For a minimum dose of four grams , it may require at least 8 to 12 capsules per day. Prescription-strength fish oil (Lovaza) is available in the United States.
An Agency for Healthcare Research and Quality (AHRQ) evidence report indicated likely benefit of omega-3 fatty acids, with regard to lowering triglyceride blood levels. Dietary sources of fish oil include fish such as trout, mackerel, herring, tuna, salmon, and sardines. Other dietary sources of omega-3 fatty acids include lean grass fed red meat, poultry, certain plant and nut oils, and omega-3 enriched products like eggs, milk, and bread. Side effects of fish oil may include burping, bad breath, heartburn, rash, upset stomach, diarrhea, and nosebleeds.
11. Zetia
Zetia is the brand name for ezetimibe. It is used in the treatment of high cholesterol and is a selective cholesterol absorption inhibitor. Zetia was approved by the United States Food and Drug Administration (FDA) in 2002 and is the only medication in its class. Zetia lowers LDL (“bad”) cholesterol levels by preventing its absorption in the small intestine. Zetia also may modestly boost HDL (“good”) cholesterol levels.
Zetia may be combined with a statin. Combining Zetia with a statin has the potential to lower LDL cholesterol levels by an average of an additional 25-percent. Side effects of Zetia may include fatigue, headache, joint pain, dizziness, cough, gallstones, pancreatitis (inflammation of the pancreas), muscle weakness, and diarrhea. There is an increased risk of liver or muscle damage when Zetia is combined with a statin. Individuals with liver disease should refrain from taking Zetia.
12. PCSK9 Inhibitors
PCSK9 inhibitors are the newest class of drug designed to treat high cholesterol. When a PCSK9 inhibitor deactivates the protein PCSK9, it enhances the absorption of LDL (“bad”) cholesterol by the liver and cholesterol levels plummet in the bloodstream. In 2015 the United States Food and Drug Administration (FDA) approved two PCSK9 inhibitors—alirocumab (Praluent) and evolocumab (Repatha). Both Praluent and Repatha can be used alone or in combination with a statin.
Three clinical trials simultaneously published in the New England Journal of Medicine concluded that PCSK9 inhibitors are extremely powerful cholesterol lowering drugs. The group administered an oral statin and PCSK9 injections every two to four weeks had 60-percent lower LDL (“bad”) cholesterol levels after one year. The fact that PCSK9 inhibitors have to be injected every two to four weeks was an inconvenience for some patients. Side effects of PCSK9 inhibitors may include confusion, difficulty concentrating, rash, and back pain.