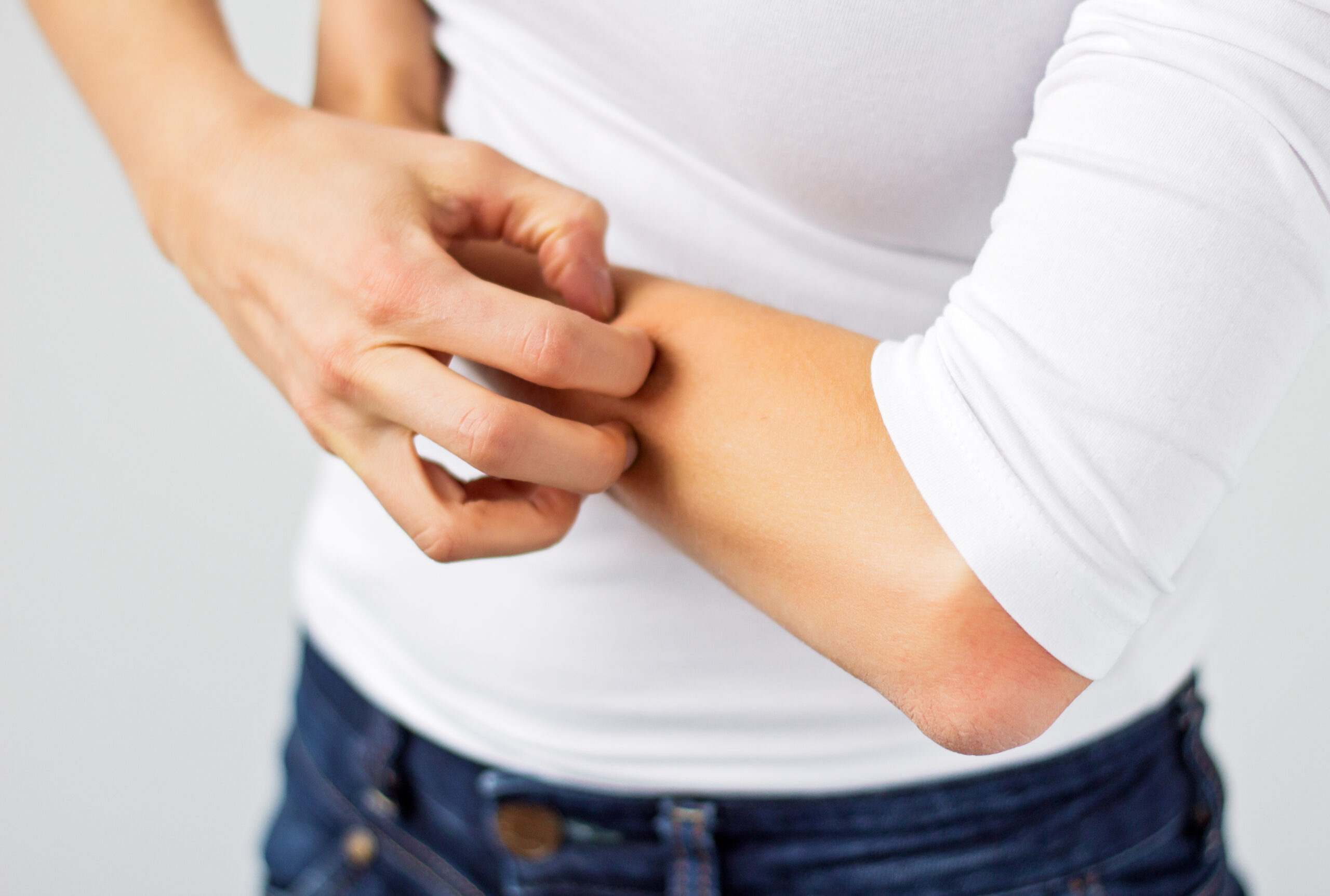
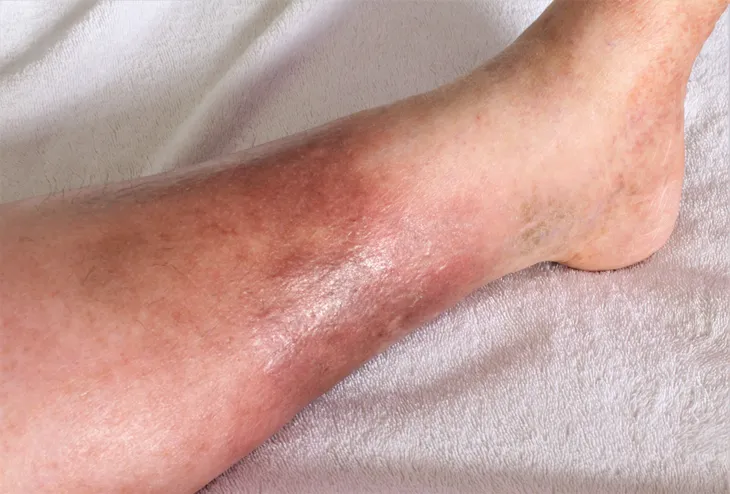
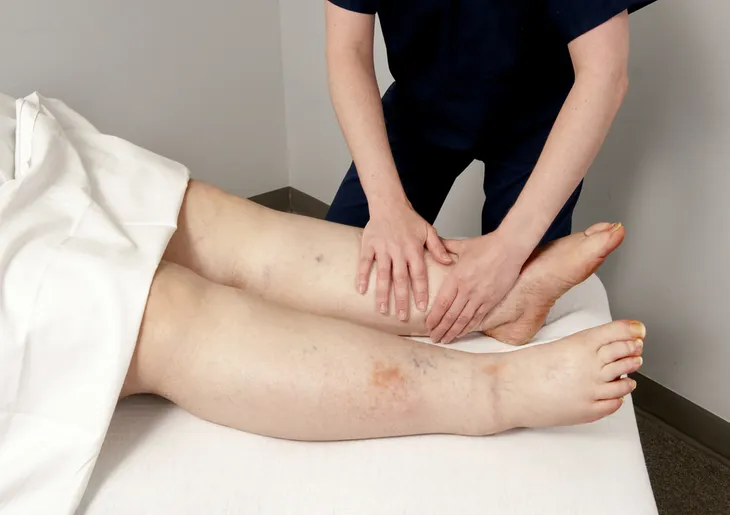
Cellulitis (not to be confused with cellulite) is a bacterial infection of the skin and is typically caused by staphylococcus or streptococcus bacteria that enters the body through an open cut or wound. It infects the deep layer of skin as well as the subcutaneous tissues, which are fat and soft tissue under the skin. Drugs.com notes that cellulitis may appear anywhere on the body, but it is most likely to occur on the legs or the arms. It appears as a red and swollen rash that will often feel warm and tender to touch.
Fortunately, it is not contagious and can be treated with antibiotics. However, if left untreated it can spread rapidly to other parts of the body and quickly become life-threatening. Here are eight facts and risk factors of cellulitis.
Want diet & nutrition content delivered straight to your inbox? Sign up for our exclusive diet & nutrition newsletter!
1. Redness and Swelling
Essentially, cellulitis is a severe rash on the skin. The Mayo Clinic notes the symptoms of cellulitis as a red and swollen area of the skin that is warm to the touch. Other symptoms include blisters or abscesses and in some cases, depending on the severity of the infection, it could be tender and a touch painful. Medicinenet.com describes the symptoms as beginning as an infected area that spreads to adjacent skin as it worsens.
Without early treatment, the symptoms could progress to a fever, chills, dizziness, nausea, and fatigue. If the condition becomes this serious, oral antibiotics might not treat the infection properly and you may require hospital treatment for intravenous (IV) antibiotics.
2. Injury
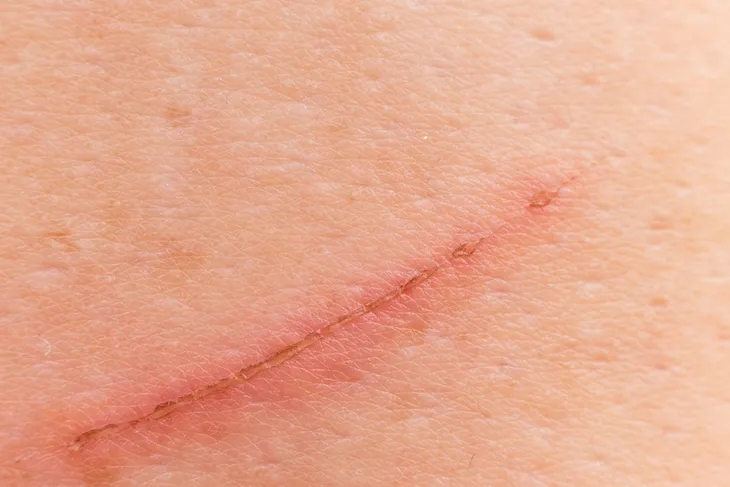
A staph infection, such as cellulitis, can develop several different ways, but what almost all of them have in common is that they are all caused by a break or cut in the skin. The Mayo Clinic notes that bacteria needs an opening to find its way under the skin to cause an infection, so anything from a scrape to a blister or a burn can be the gateway for the bacteria to enter the body.
How you treat the break in the skin will determine your likelihood of getting an infection or not.
3. Pre-Existing Skin Conditions
There are other factors that put individuals at risk for developing cellulitis. Medicinenet.com explains that if you have a pre-existing skin condition that causes breaks and tears in the skin, you could be at risk of cellulitis. People with eczema, psoriasis, chickenpox, shingles and athlete’s foot could potentially develop a more serious infection because all these conditions cause breaks or tears and result in dry and irritated skin.
It’s important to treat any of these skin conditions with the appropriate medications or ointments and to keep the skin clean to prevent infection. The healthier the skin is, the easier it will be to fight off any infection.
4. Weakened Immune System
The Mayo Clinic notes that a weakened immune system is a risk factor for developing cellulitis. Illnesses such as diabetes, leukemia, liver disease, hepatitis, or HIV/AIDS allow infections to occur easily. The source also notes that certain medications, such as corticosteroids, have the ability to weaken your immune system, allowing you to be more susceptible to infections.
A small cut might not be a big risk for someone with a strong and healthy immune system, but for someone with a weakened immune system, it could potentially be hazardous.
5. Intravenous Drug Use
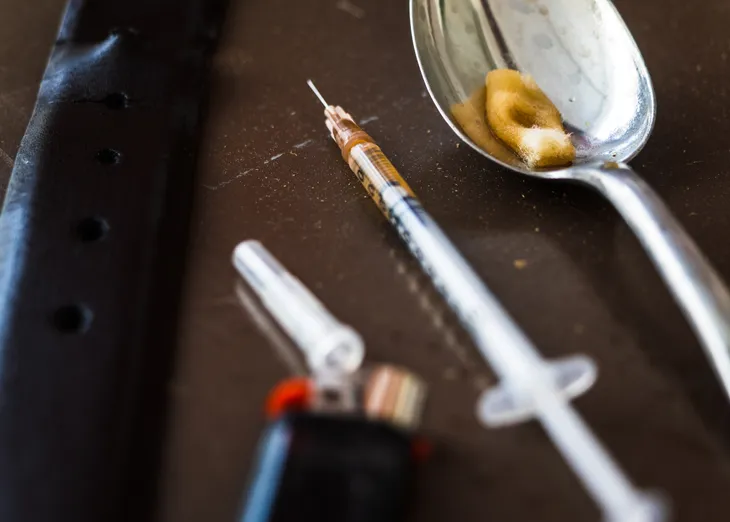
According to drugaddictiontreatment.com, IV drug users are at an increased risk of developing infections, such as cellulitis, and are also more likely to have a pre-existing condition that would weaken their immune system, increasing their risk of developing cellulitis. IV drug use could be prescribed medically and administered by a doctor or nurse, or it could be in the form of an illegal substance.
However, when receiving treatment from a medical professional, the medical tools and supplies are new and sterile, whereas someone using illegal IV drugs may not always be using the most sanitary of tools and supplies. This puts people with an IV drug addiction at a higher risk of developing cellulitis.
6. Lymphedema
Medical News Today describes lymphedema as partial or complete swelling of the legs, fingers, toes, and potentially the head or neck, which is caused by mutations in some of the genes in the lymphatic system, cancer-related treatments, or other inflammatory conditions. With inflammatory conditions such as lymphedema, the skin is more likely to crack because it is overstretched.
The source also notes that the lymphatic system is responsible for fighting infection and assists the body in defending it against bacteria. Cellulitis is a common complication for people suffering from lymphedema because the body can’t fight off infections as easily.
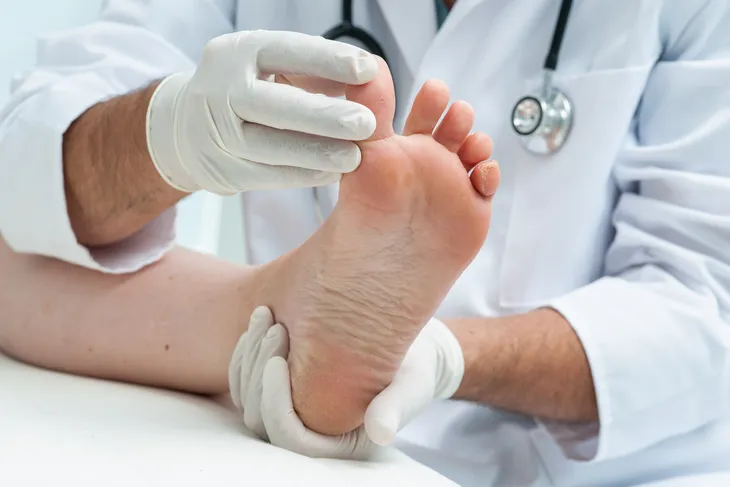
7. Athlete’s Foot
A common risk factor for cellulitis is surprisingly enough, athlete’s foot. The health website Patient.info describes athlete’s foot as a mild fungal infection that causes tiny cracks in the skin in between the toes. The way it causes cellulitis is the bacteria gets in through the cracks between the toes and travels up the leg, causing cellulitis in the calf which oddly enough, doesn’t infect the actual toes or foot. The source also notes that the cellulitis might reappear if both the infection and the athlete’s foot are treated. It’s not uncommon for this to be overlooked and for the cellulitis to reappear.
However, cellulitis is one of those conditions that, if you’ve had it once, you’re susceptible to having it again. That being said, just because you’ve had it once doesn’t guarantee that you’ll have it again — it only increases your chances of developing cellulitis. Talk to your doctor about recurrent episodes of cellulitis, in which case, you might require long-term antibiotics for prevention and recurrences of cellulitis.
8. Prevention
As you now know, there are multiple ways one can contract or develop cellulitis. However, it is easily avoidable, and there are precautions we can take to ensure you don’t develop this infection, even if you are not at high risk for developing cellulitis. It’s important to always clean and disinfect any wounds or scrapes you may get and bandage them up appropriately.
The Mayo Clinic also recommends that you keep your skin well moisturized. If the skin is soft and hydrated, it is less likely to break, which could cause an infection. It’s also important to wear the appropriate clothing and footwear when needed to protect your skin, especially if you have had cellulitis in the past.